Urgent Changes Needed to BC's Funded IVF Program


Urgent Changes Needed to BC's Funded IVF Program
The Issue
Call to Action: Improve British Columbia’s Publicly Funded IVF Program
Join us in urging the Honourable Josie Osborne, Minister of Health for the Government of British Columbia, to implement these improvements to the British Columbia’s publicly funded IVF program as soon as possible.
Firstly, many of us in the fertility community appreciate the recent launch of BC’s IVF program on July 2, 2025 [1], which marks a significant step forward in reproductive healthcare for British Columbians.
The burden of infertility and other fertility struggles (often disproportionately on women), means many of us endure profound emotional and physical distress in silence, and navigating treatment in a system with very few public supports. The roll out of this program takes a step in lifting that burden.
However, the rollout of this program needs urgent changes to be more equitable and accessible.
IVF is not a choice or a luxury, it is necessary treatment.
Infertility is a medical condition. The World Health Organization classifies infertility as a disease of the reproductive system [2] and having access to fertility treatment for conception is a human right. [3]
For couples like my husband and me with severe male factor infertility and PCOS—both congenital and beyond our control—IVF is the prescribed medical treatment with no alternative cure. The same is the case for circumstantial infertility, where reproductive care like IVF is often required because of how we were born or as a single person trying to have a child and requires assisted reproductive technology.
Under the Canada Health Act, services that are medically necessary and provided by a physician are eligible for public coverage, such as MSP in BC. IVF clearly meets these criteria, as it is administered by a specialized physician to treat a diagnosed medical condition, such as repeat pregnancy loss.
IVF is expensive but there is no alternative.
We fertility patients have exhausted other options before it leads us to IVF as the necessary last resort.
The price tag for IVF treatment in BC, regardless of whether they’re an individual or a couple, can range from $25,000 to over $150,000.
Many of us need multiple rounds of IVF to screen embryos and/or purchase donor sperm and/or donor eggs because of conditions such as Diminished Ovarian Reserve, endometriosis, or Primary Ovarian Insufficiency, or screening for a genetic condition.
In the end this is our option, IVF. Nothing else. If we don't have the finances we likely lose out on ever having a baby. That is devastating for those of us in this position.
Income testing this program excludes too many British Columbians: and needs to be removed.
It shouldn’t matter how much a patient financially earns to receive health care.
With the announcement of income testing, most people who require IVF will not receive the full $19,000.
The Province communication reads that they are, ‘supporting those who require IVF,’[3] but income testing excludes many British Columbians altogether from the program because they still can not afford it.
The is basically making the assumption that if your household earns more than $100,000 a year then you can afford your IVF healthcare. That’s just untrue in reality.
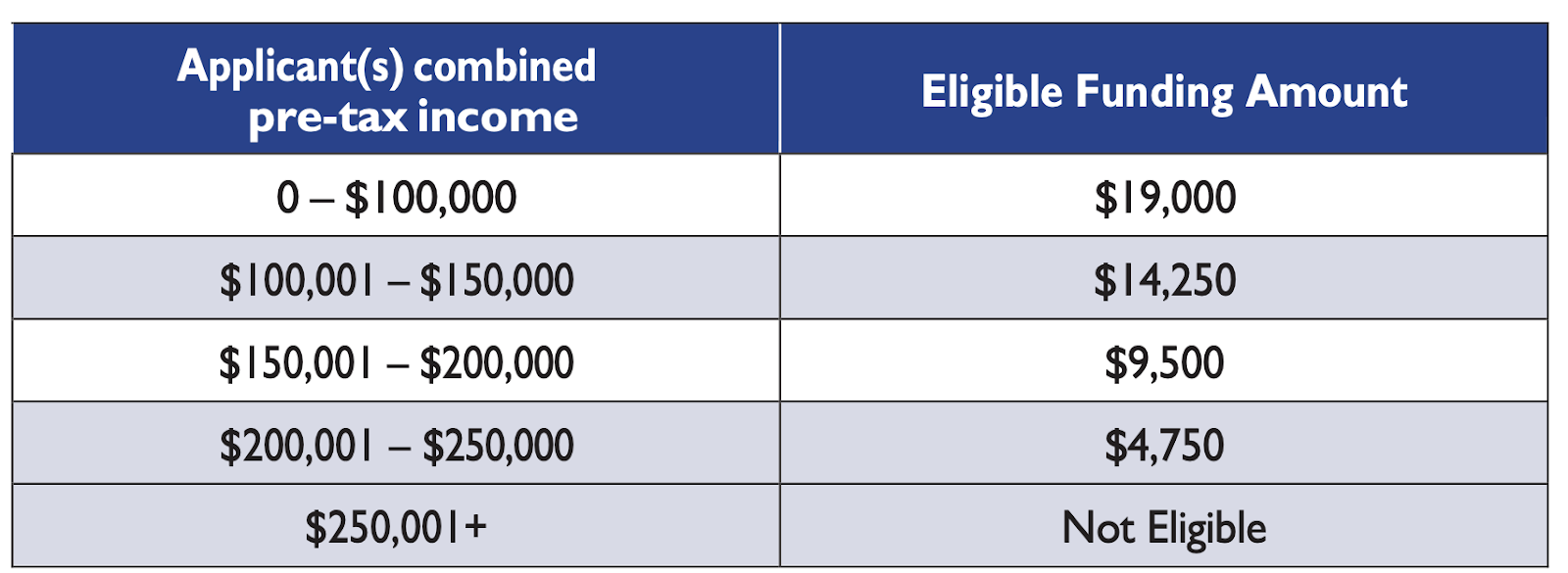
https://www2.gov.bc.ca/gov/content/health/accessing-health-care/publicly-funded-ivf-program[4]
Introducing income-based eligibility criteria suggests a misclassification of IVF as non-essential, when it is in fact medically necessary for many of us and the necessary treatment to have a baby, as stated above.
Income testing creates a form of medical gatekeeping that restricts access based on financial means rather than medical need.
IVF shouldn't be considered different that other medical procedures
If surgery to correct erectile dysfunction which is covered by MSP was income tested, there would be more outrage. It is not ethical that IVF is income tested whereas other medical procedures are not.
Income testing using CRA’s Notice of Assessment (NOA) is not the right tool
While intended to promote fairness, using last year's NOA to assess the level of support, excludes many middle-income families who still struggle to afford the high costs of IVF, which can range from $25,000 to $150,000 over the years.
Using the 2024 Notice of Assessment [1] as a basis for eligibility is also problematic because it fails to account for previously acquired wealth, investments, or family financial gifts.
The income thresholds disadvantages those who have to do multiple rounds of IVF.
Income testing disproportionately impacts those who require multiple treatment cycles or have incurred significant expenses from previous treatments.
Many fertility patients work extra hard to stay out of debt or pay off the debt they went into receiving IVF treatment in the past. These British Columbians wish that they’d worked less in 2024 in order to qualify for more in this program.
If they had known of this income tested component, a patient might have changed how they worked in 2024 or deferred paying off their previous IVF debt. I’ve heard many of these stories.
The announcement of income testing on the day of the program’s rollout was an oversight and needs to be remedied
There's an apparent misunderstanding of how fertility declines and how IVF requires intricate planning for patients. Since the announcement on March 8, 2024, many fertility patients spent 15 months planning with the understanding that the publicly funded IVF program would offer 'funded IVF' but most people learned that day that they would receive significantly less support or none at all.
This has left people in our already vulnerable fertility community feeling excluded, misled, and blindsided during a mentally and financially straining time.
In order to remedy this and to truly support those who require fertility treatment, the Province should eliminate income testing immediately.
Income testing goes against the BC Human Rights Code
People cannot be denied based on income, yet it’s excluding many and significantly impacting people’s access to this necessary treatment.
The income thresholds have lead to too many British Columbians to incur the risks of travelling abroad for IVF
Disqualifying so many British Columbians has lead to more patients seeking treatment abroad where costs are lower.
Fertility treatment abroad means accessing healthcare that may can be riskier because the health regulations differ to Canada’s. For example, Canada has successfully reduced the incidence of multiples by limiting the number of embryo transfers with multiple embryos and reducing the rate of twins and triplets through single embryo transfers.
Unfortunately many countries outside of Canada do not restrict and do not incur the consequence on their own healthcare system, but Canadians will return to BC with higher risks to the people and burdening the healthcare system.
This undermines the goal of equitable, safe access to fertility care.
BC’s IVF Program Needs to be Permanent
This program is set to run for 2 years. This leaves so much uncertainty for current patients who are far down on the wait list and for future fertility patients.
We urge Minister Osborne to extend the IVF program beyond the current two-year commitment to ensure it becomes a permanent fixture, providing stability and predictability for future fertility patients to plan around, and to address the backlog of patients who need treatment now, without imposing income restrictions.
Increase the Program Age Limit Increased from 42 to 43
Increasing the age limit from 42 to 43 would align with other provinces such as Ontario, to expand access for individuals who require fertility treatment who need it.
Excluding based on age goes against the BC Human Rights Code, especially when the need for IVF increases with age and BC has higher rates of people 40 and older accessing fertility care.
Implement A More Transparent, Patient-Centred Waitlist System
The waitlist for each clinic should be transparent. Currently, there's no way of knowing or comparing among them.
Also, the waitlist should follow the patient. The fertility clinics across British Columbia vary in terms of what each fertility doctor specializes in (endometriosis, anatomical issues), vary in terms of location of their main clinic or satellite offices, and vary based on what third party reproduction services are offered. As a result of a new diagnosis or other development, a patient may needs to switch clinics. This should be a seamless switch.
Currently, switching clinics requires a patient to lose their spot on the funded waitlist. Again, fertility declines and is time sensitive. Waiting can greatly affect the success of IVF.
To be patient-centred, we recommend that we reorganize the waitlist system so that it follows the individual rather than being tied to a specific clinic, allowing seamless transitions if a patient needs to switch providers due to diagnosis or another reason.
Fund Comprehensive Fertility & Pregnancy Loss Mental Health Supports
There is an intense and significant emotional toll when for British Columbians who face infertility, pregnancy loss, and/or IVF failure.
BC’s does not currently include any wrap-around services to support the mental health needs of IVF patients no matter whether they pay out of pocket or through the funded program. With more IVF, the need grows.
Funding programs such as Butterfly Support Network to offer free counsellor-led support groups, peer led supports, and provide guidance would meet the need of this patient population. We urge the Province to fund such programs so that patients have mental health supports, ones that are not attached to the clinics where patients can be met without judgement or any conflict of interest.
Conclusion
British Columbia’s fertility community deserves an IVF program that is accessible, equitable, and compassionate. Removing barriers such as income testing and expanding support will ensure that all individuals and couples across BC have the opportunity to build their families with dignity and care.
Sincerely,
Laura Spencer
BC resident, IVF patient, certified fertility coach
References:
[1] Government of British Columbia website (July 2, 2025) https://www2.gov.bc.ca/gov/content/health/accessing-health-care/publicly-funded-ivf-program
[2] Zegers‐Hochschild, F., Adamson, G. D., de Mouzon, J., Ishihara, O., Mansour, R., Nygren, K., … Vanderpoel, S. (2009). International Committee for Monitoring Assisted Reproductive Technology (ICMART) and the World Health Organization (WHO) revised glossary of ART terminology, 2009. Fertility and Sterility, 92, 1520–1524: 1522.
[3] Zegers‐Hochschild F, Dickens BM, Dughman‐Manzur S. Human rights to in vitro fertilization. International Journal of Gynecology & Obstetrics 2013;123(1):86-89.
[4] BC Publicly Funded IVF Program Patient Information Sheet https://www2.gov.bc.ca/assets/gov/health/accessing-health-care/publicly-funded-ivf-program/10527_ivf_factsheet_v7_final.pdf
448
The Issue
Call to Action: Improve British Columbia’s Publicly Funded IVF Program
Join us in urging the Honourable Josie Osborne, Minister of Health for the Government of British Columbia, to implement these improvements to the British Columbia’s publicly funded IVF program as soon as possible.
Firstly, many of us in the fertility community appreciate the recent launch of BC’s IVF program on July 2, 2025 [1], which marks a significant step forward in reproductive healthcare for British Columbians.
The burden of infertility and other fertility struggles (often disproportionately on women), means many of us endure profound emotional and physical distress in silence, and navigating treatment in a system with very few public supports. The roll out of this program takes a step in lifting that burden.
However, the rollout of this program needs urgent changes to be more equitable and accessible.
IVF is not a choice or a luxury, it is necessary treatment.
Infertility is a medical condition. The World Health Organization classifies infertility as a disease of the reproductive system [2] and having access to fertility treatment for conception is a human right. [3]
For couples like my husband and me with severe male factor infertility and PCOS—both congenital and beyond our control—IVF is the prescribed medical treatment with no alternative cure. The same is the case for circumstantial infertility, where reproductive care like IVF is often required because of how we were born or as a single person trying to have a child and requires assisted reproductive technology.
Under the Canada Health Act, services that are medically necessary and provided by a physician are eligible for public coverage, such as MSP in BC. IVF clearly meets these criteria, as it is administered by a specialized physician to treat a diagnosed medical condition, such as repeat pregnancy loss.
IVF is expensive but there is no alternative.
We fertility patients have exhausted other options before it leads us to IVF as the necessary last resort.
The price tag for IVF treatment in BC, regardless of whether they’re an individual or a couple, can range from $25,000 to over $150,000.
Many of us need multiple rounds of IVF to screen embryos and/or purchase donor sperm and/or donor eggs because of conditions such as Diminished Ovarian Reserve, endometriosis, or Primary Ovarian Insufficiency, or screening for a genetic condition.
In the end this is our option, IVF. Nothing else. If we don't have the finances we likely lose out on ever having a baby. That is devastating for those of us in this position.
Income testing this program excludes too many British Columbians: and needs to be removed.
It shouldn’t matter how much a patient financially earns to receive health care.
With the announcement of income testing, most people who require IVF will not receive the full $19,000.
The Province communication reads that they are, ‘supporting those who require IVF,’[3] but income testing excludes many British Columbians altogether from the program because they still can not afford it.
The is basically making the assumption that if your household earns more than $100,000 a year then you can afford your IVF healthcare. That’s just untrue in reality.

https://www2.gov.bc.ca/gov/content/health/accessing-health-care/publicly-funded-ivf-program[4]
Introducing income-based eligibility criteria suggests a misclassification of IVF as non-essential, when it is in fact medically necessary for many of us and the necessary treatment to have a baby, as stated above.
Income testing creates a form of medical gatekeeping that restricts access based on financial means rather than medical need.
IVF shouldn't be considered different that other medical procedures
If surgery to correct erectile dysfunction which is covered by MSP was income tested, there would be more outrage. It is not ethical that IVF is income tested whereas other medical procedures are not.
Income testing using CRA’s Notice of Assessment (NOA) is not the right tool
While intended to promote fairness, using last year's NOA to assess the level of support, excludes many middle-income families who still struggle to afford the high costs of IVF, which can range from $25,000 to $150,000 over the years.
Using the 2024 Notice of Assessment [1] as a basis for eligibility is also problematic because it fails to account for previously acquired wealth, investments, or family financial gifts.
The income thresholds disadvantages those who have to do multiple rounds of IVF.
Income testing disproportionately impacts those who require multiple treatment cycles or have incurred significant expenses from previous treatments.
Many fertility patients work extra hard to stay out of debt or pay off the debt they went into receiving IVF treatment in the past. These British Columbians wish that they’d worked less in 2024 in order to qualify for more in this program.
If they had known of this income tested component, a patient might have changed how they worked in 2024 or deferred paying off their previous IVF debt. I’ve heard many of these stories.
The announcement of income testing on the day of the program’s rollout was an oversight and needs to be remedied
There's an apparent misunderstanding of how fertility declines and how IVF requires intricate planning for patients. Since the announcement on March 8, 2024, many fertility patients spent 15 months planning with the understanding that the publicly funded IVF program would offer 'funded IVF' but most people learned that day that they would receive significantly less support or none at all.
This has left people in our already vulnerable fertility community feeling excluded, misled, and blindsided during a mentally and financially straining time.
In order to remedy this and to truly support those who require fertility treatment, the Province should eliminate income testing immediately.
Income testing goes against the BC Human Rights Code
People cannot be denied based on income, yet it’s excluding many and significantly impacting people’s access to this necessary treatment.
The income thresholds have lead to too many British Columbians to incur the risks of travelling abroad for IVF
Disqualifying so many British Columbians has lead to more patients seeking treatment abroad where costs are lower.
Fertility treatment abroad means accessing healthcare that may can be riskier because the health regulations differ to Canada’s. For example, Canada has successfully reduced the incidence of multiples by limiting the number of embryo transfers with multiple embryos and reducing the rate of twins and triplets through single embryo transfers.
Unfortunately many countries outside of Canada do not restrict and do not incur the consequence on their own healthcare system, but Canadians will return to BC with higher risks to the people and burdening the healthcare system.
This undermines the goal of equitable, safe access to fertility care.
BC’s IVF Program Needs to be Permanent
This program is set to run for 2 years. This leaves so much uncertainty for current patients who are far down on the wait list and for future fertility patients.
We urge Minister Osborne to extend the IVF program beyond the current two-year commitment to ensure it becomes a permanent fixture, providing stability and predictability for future fertility patients to plan around, and to address the backlog of patients who need treatment now, without imposing income restrictions.
Increase the Program Age Limit Increased from 42 to 43
Increasing the age limit from 42 to 43 would align with other provinces such as Ontario, to expand access for individuals who require fertility treatment who need it.
Excluding based on age goes against the BC Human Rights Code, especially when the need for IVF increases with age and BC has higher rates of people 40 and older accessing fertility care.
Implement A More Transparent, Patient-Centred Waitlist System
The waitlist for each clinic should be transparent. Currently, there's no way of knowing or comparing among them.
Also, the waitlist should follow the patient. The fertility clinics across British Columbia vary in terms of what each fertility doctor specializes in (endometriosis, anatomical issues), vary in terms of location of their main clinic or satellite offices, and vary based on what third party reproduction services are offered. As a result of a new diagnosis or other development, a patient may needs to switch clinics. This should be a seamless switch.
Currently, switching clinics requires a patient to lose their spot on the funded waitlist. Again, fertility declines and is time sensitive. Waiting can greatly affect the success of IVF.
To be patient-centred, we recommend that we reorganize the waitlist system so that it follows the individual rather than being tied to a specific clinic, allowing seamless transitions if a patient needs to switch providers due to diagnosis or another reason.
Fund Comprehensive Fertility & Pregnancy Loss Mental Health Supports
There is an intense and significant emotional toll when for British Columbians who face infertility, pregnancy loss, and/or IVF failure.
BC’s does not currently include any wrap-around services to support the mental health needs of IVF patients no matter whether they pay out of pocket or through the funded program. With more IVF, the need grows.
Funding programs such as Butterfly Support Network to offer free counsellor-led support groups, peer led supports, and provide guidance would meet the need of this patient population. We urge the Province to fund such programs so that patients have mental health supports, ones that are not attached to the clinics where patients can be met without judgement or any conflict of interest.
Conclusion
British Columbia’s fertility community deserves an IVF program that is accessible, equitable, and compassionate. Removing barriers such as income testing and expanding support will ensure that all individuals and couples across BC have the opportunity to build their families with dignity and care.
Sincerely,
Laura Spencer
BC resident, IVF patient, certified fertility coach
References:
[1] Government of British Columbia website (July 2, 2025) https://www2.gov.bc.ca/gov/content/health/accessing-health-care/publicly-funded-ivf-program
[2] Zegers‐Hochschild, F., Adamson, G. D., de Mouzon, J., Ishihara, O., Mansour, R., Nygren, K., … Vanderpoel, S. (2009). International Committee for Monitoring Assisted Reproductive Technology (ICMART) and the World Health Organization (WHO) revised glossary of ART terminology, 2009. Fertility and Sterility, 92, 1520–1524: 1522.
[3] Zegers‐Hochschild F, Dickens BM, Dughman‐Manzur S. Human rights to in vitro fertilization. International Journal of Gynecology & Obstetrics 2013;123(1):86-89.
[4] BC Publicly Funded IVF Program Patient Information Sheet https://www2.gov.bc.ca/assets/gov/health/accessing-health-care/publicly-funded-ivf-program/10527_ivf_factsheet_v7_final.pdf
448
The Decision Makers
Supporter Voices
Petition Updates
Share this petition
Petition created on July 19, 2025