Monopoly? You Keep Using That Word:A Recipient Moms View on the US Organ Allocation System

Monopoly? You Keep Using That Word:A Recipient Moms View on the US Organ Allocation System
The Issue
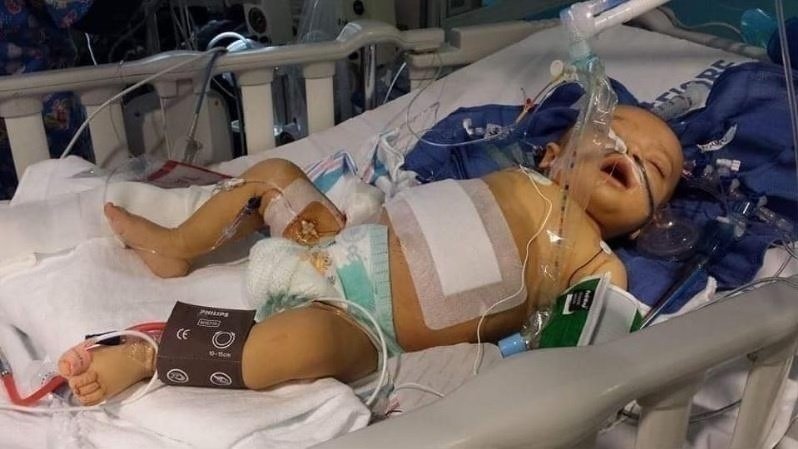
Caption: Caleb Munn, pediatric liver recipient
“Monopoly?” You Keep Using That Word: A Pediatric Transplant Recipient Mom’s View on the U.S. Organ Allocation System
By Brittany Munn, Co-Chair, Patient Family Engaged Partners, Society of Pediatric Liver Transplantation
The word “Monopoly” continues to be used in many of the latest articles about our current organ allocation system and UNOS. As a mother of a pediatric liver transplant recipient, this comparison makes me laugh, and reminds me of a line in the movie The Princess Bride, when Vizzini keeps using the word “inconceivable!” and Inigo Montoya replies, “You keep using that word. I do not think it means what you think it means.” For example, in the recent article, “Monopoly Be Gone: A New Chapter in U.S. Organ Procurement and Transplantation” by Greg Segal, Jennifer Erickson, MS, Donna Cryer, JD, and Bryan Sivak states, “The U.S. government recently made a transformative announcement: it is breaking up the flawed monopoly that manages the current organ procurement system, the Organ Procurement and Transplantation Network (OPTN).” This opening statement alone is a perfect example of how misunderstood our current organ transplant system is. Our organ allocation system is most definitely flawed. I learned firsthand after my son was diagnosed with a rare liver disease at the age of four months old in 2015. As a nation, we are better off improving our current system to serve patients and families in a more effective way. Eliminating UNOS, and then starting from scratch, isn’t the answer in my opinion. Though, in order to fix what we have, we need to understand how it functions first.
Currently, our organ transplant system is made up of nonprofit organizations working hand in hand to help save thousands of lives. UNOS (United Network for Organ Sharing), OPTN (Organ Procurement and Transplantation Network), local OPOs (Organ Procurement Organizations), and transplant hospitals all work together to share and transplant organs across the nation. According to the UNOS website, UNOS “manages the national transplant waiting list, matching donors to recipients 24 hours a day, 365 days a year, through UNet technology used by organ donation and transplant professionals every day to save lives through transplantation. UNOS is the non-profit organization that built and continuously improves UNet in partnership with innovative technology tools and partners. UNOS continues to accomplish this through policy updates, education and technology.”
Policy updates are actually done through the Organ Procurement and Transplant Network (OPTN). Once ideas have been gathered to better the policies of transplantation, OPTN will develop and evaluate potential solutions for projects. OPTN’s website states, “The OPTN acts through its Board of Directors and committees, who bring a wealth of commitment and technical knowledge to guide us. Committees address issues of concern in the transplant community. The board establishes and maintains transplant policies (operational rules) and bylaws (membership requirements) that govern the OPTN. It is a unique public-private partnership that links all professionals involved in the U.S. donation and transplantation system.” UNOS committees and Board of Directors help make policies for OPTN, with a participatory process from stakeholders in the community. The collaboration within the OPTN allows all members of the transplantation process in this country to weigh in on these policies. OPTN members consist of transplant centers, histocompatibility laboratories, public organizations, individual members, medical scientific organizations, business members, and all 56 OPOs.
After the OPTN creates and handles the policies, and UNOS helps match donors to recipients, our local OPOs handle the delicate process of retrieving the donated organs and placing them with the transplant surgeons whom they were matched with. OPOs meet with the donor families and hold their hand every step of the way if a loved one is donating their organs. I personally find these front-line organizations to be quite remarkable. I am a volunteer at my local OPO, ConnectLife, and the more I learn about them, the more I am in awe at what these wonderful people do 24 hours a day, 7 days a week. It is a very emotional, but rewarding job.
Once the OPOs help place the donated organs, it is our transplant hospitals that make the final call on whether or not those organs are viable and can be transplanted into a recipient. This is one of the most misunderstood parts of the whole process. UNOS is blamed for all discarded organs, however, if an organ makes it to a matched recipient, their transplant surgeon (and in some cases, even the transplant recipient) has the final say in the end. There are many factors that go into accepting and transplanting an organ. According to the article on National Library of Medicine, “Accepting a Donor Kidney: an Evaluation of Patients’ and Transplant Surgeons’ Priorities”, by Daniel A. Solomon, Nicole Rabidou, Sanjay Kulkarni, Richard Formica, and Liana Fraenkel, “There are, however, two elements of the decision that validate declining the kidney as a reasonable alternative: change in patient characteristics over time, and heterogeneity of donor kidneys- baseline function, risk of contracting a disease, likelihood of rejection, and expected graft survival time. In addition, a zero-antigen mismatched kidney has a lower risk of rejection and greater overall graft survival. Thus, a patient may choose to minimize the risk of graft rejection, and maximize the chance of graft survival, by holding out for a kidney that is a closer match and of higher quality.” These elements are used for every organ being transplanted, not just kidneys, and if a matched organ makes its way to a transplant hospital, once the surgeon evaluates it in person, one of these factors could have the surgeon ultimately rejecting the organ. If that decision is made at the final evaluation, this can cause organs to be discarded due to time restraints, meaning a refused organ for one potential match may no longer reach another potential match in time. According to donatelife.org, a Lung has 4 to 6 hours of life outside the body, a Heart is up to 4 hours, Liver and Pancreas have up to 24 hours of life, and Kidneys have the longest lifespan of 72 hours. Time is of the essence once the donation has occurred, and unfortunately, if an organ doesn’t meet a certain standard for a transplant surgeon, those organs may no longer be transplantable.
As you can see, our transplant system here in the U.S. is made up of many non-profit organizations all working together to save lives. If I am not mistaken, the definition of monopoly is “a business that is the only seller of a good or service.” UNOS might be helping connect all of these organizations, but it is not controlling the entire process from beginning to end, and it is not selling organs for profit.
What do we do to improve what we have, and help save more lives? First, we should be more involved with the policy process right from the start. According to the OPTN website, “Public comment is an essential part of the policy development process that occurs twice each year. The OPTN policy development process incorporates public comment feedback on policy and bylaws proposals before they go to the OPTN board of directors for approval. All interested individuals are welcome to participate, especially transplant candidates, who are most affected by policies. Transplant professionals are encouraged to provide comments about potential financial impact a proposal could have on their organization.” Second, we should create better policies that put children first. According to a study that came out in September 2018, children who need lifesaving liver transplants are losing out to adults. An NBC News article that year said, “The research team examined the cases of more than 4,000 children listed for liver transplants from 2002 to 2014, and then followed up through 2016. Over that time, about 400 children died while waiting for a transplant.” My son was transplanted at 6 months old with a liver in March 2015, and thankfully he was one who survived. However, I painfully witnessed many other families I had become acquainted with during our transplant journey lose their children to rare liver diseases due to the long waitlist wait. Also stated within that same article it says, “Approximately 500 deceased-donor liver transplants are performed each year in children in the United States, a number that has remained constant over the past two decades, while the number of adults who receive transplants is more than tenfold higher and is increasing by 10 percent per year… Children must almost always get organs from other children, while adults are eligible to get organs from other adults and from children.” When you have adults removing pediatric donor livers (or kidneys) from potential children recipients, you are only increasing the odds that the child on the waitlist dies. Third, the way we view organ donation should be flipped inside out, and instead of an “opt in'' system like we currently have for people registering to be organ donors, we should have an “opt out” system, allowing UNOS, OPTN, OPOs, and transplant hospitals to have more opportunity to transplant sick patients. The public can still be given the choice, but it could allow for more organs to be available, and less people would die waiting for their second chance at life.
In the transplant community, our hope is to see our nation work together to improve the process we have now, and first and foremost, prioritize children. We saw an increase of 3.7% in transplants performed in 2022 from 2021, which was a new annual record. This tells us that our current system is working, even if it is a slow process. Now let’s just improve it! We should stop politicizing medical procedures in this country, and start actually doing something that will better the lives of those waiting for a second chance at life. We need to start thinking of the children first when it comes to creating the policies that shape our transplant system. No child should be left without a viable organ option!
Citations:
“Monopoly Be Gone: A New Chapter in U.S. Organ Procurement and Transplantation” - by Greg Segal, Jennifer Erickson, MS, Donna Cryer, JD, and Bryan Sivak - https://www.medpagetoday.com/opinion/second-opinions/103855
UNOS- https://unos.org/about/
OPTN- https://optn.transplant.hrsa.gov/about/
Donate Life India - https://www.donatelife.org.in/time-of-organ-donation
NBC News- https://www.nbcnews.com/health/health-news/children-lose-out-liver-transplants-study-finds-n910246
“Accepting a Donor Kidney: an Evaluation of Patients’ and Transplant Surgeons’ Priorities” - by Daniel A. Solomon, Nicole Rabidou, Sanjay Kulkarni, Richard Formica, and Liana Fraenkel - https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4846340/
_________________________________________________
Signed,
Brittany Munn
Co-Chair
Patient & Family Engaged Partners of SPLIT
Mother of a liver transplant recipient
Jennifer White
Co-Chair
Patient & Family Engaged Partners of SPLIT
Mother of a liver transplant recipient
Anna Beeman
CEO
Liver Mommas & Families, Inc.
Mother of a liver transplant recipient
Jordan Sarbaugh
Co-Founder/VP
BARE Inc NFP
Mother of a liver transplant recipient
Serena Fellers
Member
Patient & Family Engaged Partners of SPLIT
Mother of a liver transplant recipient
Katy Terweele
Member
Patient & Family Engaged Partners of SPLIT
Mother of a liver transplant recipient
Sherrie Logan
Member
Patient & Family Engaged Partners of SPLIT
Mother of liver transplant recipient
Erin Babin
Member
Patient & Family Engaged Partners of SPLIT
Mother of a liver transplant recipient
Vanessa Smith
Member
Patient & Family Engaged Partners of SPLIT
Mother to a liver transplant recipient
Living Donor
Joseph P. Hillenburg
Strategy Advisor, Transplant Families
Former member, OPTN/UNOS Board of Directors
Father to a heart transplant recipient
Ansara Piebenga
Board Member, Transplant Families
Mother to a kidney and liver transplant recipient
Stacy Hillenburg
Board Member, Transplant Families
Mother to a heart transplant recipient
Jill Brown
Board Member, Transplant Families
Mother to a kidney transplant recipient
Riki Graves
Board Member, Transplant Families
Mother to a heart transplant recipient
Leslie Wyers
Co-Chair, Improving Renal Outcomes Collaborative (IROC)'s Community Engagement Workgroup (CEW)
Founder, NephHope Foundation
Former member of UNOS' Patient Affairs Committee
Living donor and mother of two kidney transplant recipients

385
The Issue
Caption: Caleb Munn, pediatric liver recipient
“Monopoly?” You Keep Using That Word: A Pediatric Transplant Recipient Mom’s View on the U.S. Organ Allocation System
By Brittany Munn, Co-Chair, Patient Family Engaged Partners, Society of Pediatric Liver Transplantation
The word “Monopoly” continues to be used in many of the latest articles about our current organ allocation system and UNOS. As a mother of a pediatric liver transplant recipient, this comparison makes me laugh, and reminds me of a line in the movie The Princess Bride, when Vizzini keeps using the word “inconceivable!” and Inigo Montoya replies, “You keep using that word. I do not think it means what you think it means.” For example, in the recent article, “Monopoly Be Gone: A New Chapter in U.S. Organ Procurement and Transplantation” by Greg Segal, Jennifer Erickson, MS, Donna Cryer, JD, and Bryan Sivak states, “The U.S. government recently made a transformative announcement: it is breaking up the flawed monopoly that manages the current organ procurement system, the Organ Procurement and Transplantation Network (OPTN).” This opening statement alone is a perfect example of how misunderstood our current organ transplant system is. Our organ allocation system is most definitely flawed. I learned firsthand after my son was diagnosed with a rare liver disease at the age of four months old in 2015. As a nation, we are better off improving our current system to serve patients and families in a more effective way. Eliminating UNOS, and then starting from scratch, isn’t the answer in my opinion. Though, in order to fix what we have, we need to understand how it functions first.
Currently, our organ transplant system is made up of nonprofit organizations working hand in hand to help save thousands of lives. UNOS (United Network for Organ Sharing), OPTN (Organ Procurement and Transplantation Network), local OPOs (Organ Procurement Organizations), and transplant hospitals all work together to share and transplant organs across the nation. According to the UNOS website, UNOS “manages the national transplant waiting list, matching donors to recipients 24 hours a day, 365 days a year, through UNet technology used by organ donation and transplant professionals every day to save lives through transplantation. UNOS is the non-profit organization that built and continuously improves UNet in partnership with innovative technology tools and partners. UNOS continues to accomplish this through policy updates, education and technology.”
Policy updates are actually done through the Organ Procurement and Transplant Network (OPTN). Once ideas have been gathered to better the policies of transplantation, OPTN will develop and evaluate potential solutions for projects. OPTN’s website states, “The OPTN acts through its Board of Directors and committees, who bring a wealth of commitment and technical knowledge to guide us. Committees address issues of concern in the transplant community. The board establishes and maintains transplant policies (operational rules) and bylaws (membership requirements) that govern the OPTN. It is a unique public-private partnership that links all professionals involved in the U.S. donation and transplantation system.” UNOS committees and Board of Directors help make policies for OPTN, with a participatory process from stakeholders in the community. The collaboration within the OPTN allows all members of the transplantation process in this country to weigh in on these policies. OPTN members consist of transplant centers, histocompatibility laboratories, public organizations, individual members, medical scientific organizations, business members, and all 56 OPOs.
After the OPTN creates and handles the policies, and UNOS helps match donors to recipients, our local OPOs handle the delicate process of retrieving the donated organs and placing them with the transplant surgeons whom they were matched with. OPOs meet with the donor families and hold their hand every step of the way if a loved one is donating their organs. I personally find these front-line organizations to be quite remarkable. I am a volunteer at my local OPO, ConnectLife, and the more I learn about them, the more I am in awe at what these wonderful people do 24 hours a day, 7 days a week. It is a very emotional, but rewarding job.
Once the OPOs help place the donated organs, it is our transplant hospitals that make the final call on whether or not those organs are viable and can be transplanted into a recipient. This is one of the most misunderstood parts of the whole process. UNOS is blamed for all discarded organs, however, if an organ makes it to a matched recipient, their transplant surgeon (and in some cases, even the transplant recipient) has the final say in the end. There are many factors that go into accepting and transplanting an organ. According to the article on National Library of Medicine, “Accepting a Donor Kidney: an Evaluation of Patients’ and Transplant Surgeons’ Priorities”, by Daniel A. Solomon, Nicole Rabidou, Sanjay Kulkarni, Richard Formica, and Liana Fraenkel, “There are, however, two elements of the decision that validate declining the kidney as a reasonable alternative: change in patient characteristics over time, and heterogeneity of donor kidneys- baseline function, risk of contracting a disease, likelihood of rejection, and expected graft survival time. In addition, a zero-antigen mismatched kidney has a lower risk of rejection and greater overall graft survival. Thus, a patient may choose to minimize the risk of graft rejection, and maximize the chance of graft survival, by holding out for a kidney that is a closer match and of higher quality.” These elements are used for every organ being transplanted, not just kidneys, and if a matched organ makes its way to a transplant hospital, once the surgeon evaluates it in person, one of these factors could have the surgeon ultimately rejecting the organ. If that decision is made at the final evaluation, this can cause organs to be discarded due to time restraints, meaning a refused organ for one potential match may no longer reach another potential match in time. According to donatelife.org, a Lung has 4 to 6 hours of life outside the body, a Heart is up to 4 hours, Liver and Pancreas have up to 24 hours of life, and Kidneys have the longest lifespan of 72 hours. Time is of the essence once the donation has occurred, and unfortunately, if an organ doesn’t meet a certain standard for a transplant surgeon, those organs may no longer be transplantable.
As you can see, our transplant system here in the U.S. is made up of many non-profit organizations all working together to save lives. If I am not mistaken, the definition of monopoly is “a business that is the only seller of a good or service.” UNOS might be helping connect all of these organizations, but it is not controlling the entire process from beginning to end, and it is not selling organs for profit.
What do we do to improve what we have, and help save more lives? First, we should be more involved with the policy process right from the start. According to the OPTN website, “Public comment is an essential part of the policy development process that occurs twice each year. The OPTN policy development process incorporates public comment feedback on policy and bylaws proposals before they go to the OPTN board of directors for approval. All interested individuals are welcome to participate, especially transplant candidates, who are most affected by policies. Transplant professionals are encouraged to provide comments about potential financial impact a proposal could have on their organization.” Second, we should create better policies that put children first. According to a study that came out in September 2018, children who need lifesaving liver transplants are losing out to adults. An NBC News article that year said, “The research team examined the cases of more than 4,000 children listed for liver transplants from 2002 to 2014, and then followed up through 2016. Over that time, about 400 children died while waiting for a transplant.” My son was transplanted at 6 months old with a liver in March 2015, and thankfully he was one who survived. However, I painfully witnessed many other families I had become acquainted with during our transplant journey lose their children to rare liver diseases due to the long waitlist wait. Also stated within that same article it says, “Approximately 500 deceased-donor liver transplants are performed each year in children in the United States, a number that has remained constant over the past two decades, while the number of adults who receive transplants is more than tenfold higher and is increasing by 10 percent per year… Children must almost always get organs from other children, while adults are eligible to get organs from other adults and from children.” When you have adults removing pediatric donor livers (or kidneys) from potential children recipients, you are only increasing the odds that the child on the waitlist dies. Third, the way we view organ donation should be flipped inside out, and instead of an “opt in'' system like we currently have for people registering to be organ donors, we should have an “opt out” system, allowing UNOS, OPTN, OPOs, and transplant hospitals to have more opportunity to transplant sick patients. The public can still be given the choice, but it could allow for more organs to be available, and less people would die waiting for their second chance at life.
In the transplant community, our hope is to see our nation work together to improve the process we have now, and first and foremost, prioritize children. We saw an increase of 3.7% in transplants performed in 2022 from 2021, which was a new annual record. This tells us that our current system is working, even if it is a slow process. Now let’s just improve it! We should stop politicizing medical procedures in this country, and start actually doing something that will better the lives of those waiting for a second chance at life. We need to start thinking of the children first when it comes to creating the policies that shape our transplant system. No child should be left without a viable organ option!
Citations:
“Monopoly Be Gone: A New Chapter in U.S. Organ Procurement and Transplantation” - by Greg Segal, Jennifer Erickson, MS, Donna Cryer, JD, and Bryan Sivak - https://www.medpagetoday.com/opinion/second-opinions/103855
UNOS- https://unos.org/about/
OPTN- https://optn.transplant.hrsa.gov/about/
Donate Life India - https://www.donatelife.org.in/time-of-organ-donation
NBC News- https://www.nbcnews.com/health/health-news/children-lose-out-liver-transplants-study-finds-n910246
“Accepting a Donor Kidney: an Evaluation of Patients’ and Transplant Surgeons’ Priorities” - by Daniel A. Solomon, Nicole Rabidou, Sanjay Kulkarni, Richard Formica, and Liana Fraenkel - https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4846340/
_________________________________________________
Signed,
Brittany Munn
Co-Chair
Patient & Family Engaged Partners of SPLIT
Mother of a liver transplant recipient
Jennifer White
Co-Chair
Patient & Family Engaged Partners of SPLIT
Mother of a liver transplant recipient
Anna Beeman
CEO
Liver Mommas & Families, Inc.
Mother of a liver transplant recipient
Jordan Sarbaugh
Co-Founder/VP
BARE Inc NFP
Mother of a liver transplant recipient
Serena Fellers
Member
Patient & Family Engaged Partners of SPLIT
Mother of a liver transplant recipient
Katy Terweele
Member
Patient & Family Engaged Partners of SPLIT
Mother of a liver transplant recipient
Sherrie Logan
Member
Patient & Family Engaged Partners of SPLIT
Mother of liver transplant recipient
Erin Babin
Member
Patient & Family Engaged Partners of SPLIT
Mother of a liver transplant recipient
Vanessa Smith
Member
Patient & Family Engaged Partners of SPLIT
Mother to a liver transplant recipient
Living Donor
Joseph P. Hillenburg
Strategy Advisor, Transplant Families
Former member, OPTN/UNOS Board of Directors
Father to a heart transplant recipient
Ansara Piebenga
Board Member, Transplant Families
Mother to a kidney and liver transplant recipient
Stacy Hillenburg
Board Member, Transplant Families
Mother to a heart transplant recipient
Jill Brown
Board Member, Transplant Families
Mother to a kidney transplant recipient
Riki Graves
Board Member, Transplant Families
Mother to a heart transplant recipient
Leslie Wyers
Co-Chair, Improving Renal Outcomes Collaborative (IROC)'s Community Engagement Workgroup (CEW)
Founder, NephHope Foundation
Former member of UNOS' Patient Affairs Committee
Living donor and mother of two kidney transplant recipients

385
Petition Updates
Share this petition
Petition created on May 18, 2023


