Individuals’ Right under HIPAA to Access their Health Information 45 CFR § 164.524


Individuals’ Right under HIPAA to Access their Health Information 45 CFR § 164.524
The Issue
Individuals’ Right under HIPAA to Access their Health Information 45 CFR § 164.524
Patients' rights are detailed in the Health Insurance Portability and Accountability Act (HIPAA) which states that individuals have a legal right to obtain copies of their health data stored by their healthcare providers.
Patient Rights – WMA – The World Medical Association
Additional Relevant Assembly Info, Located at the End Portion of this Petition.
Personal difficulties are present in gaining access to medical records, particularly of Radiology Reports & an ER report. The traditional request for records method(s) took place, returning results of "patient not found" or replies of "all records provided" with referrals to obtain in alternate ways. Technical encounters are frequent amidst, the numerous ways of which to attempt to obtain them via instruction(s) and have been reported to the associated technology companies of affiliation with the health facilities and/or practitioners.
UPMC, Pennsylvania and an additional system, VHC, Virginia are two medical networks where numerous complications of obtaining records have taken place in recent years. Despite bringing this to the attention of health regulation and standards organizations including the American Medical Association (AMA), the American Health Association (AHA), the Council for State Governments (CSG), the International Joint Commission (IJC), the World Medical Association (WMA), and United Nations affiliates, radiology reports from initial injury sustained date, have not been released.
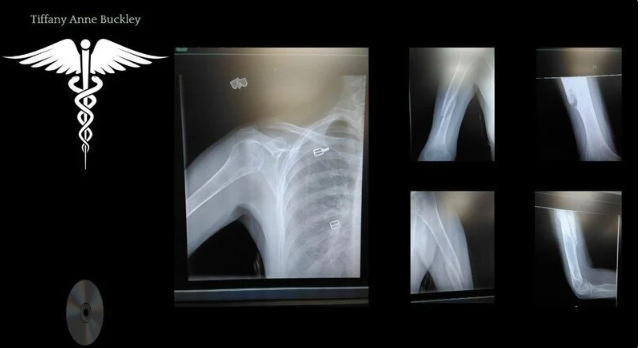
The statute of limitations passed for the incident date of 02/05/2023 to attempt for any settlement, claims or actions. Physicians indicated within the reports, a spiral fracture of the humerus bone, yet markers indicate from the X-Rays that other areas, may have been affected and not included in the description of incidence. These photos are from 9 months post the original injury. Obtaining the ER Report from the date of incidence on 02/05/2023 and the radiology reports taken while in the state of PA, from Feb - Aug of 2023, is the reason for this request for support.
The radiology image shown here, appears to indicate injuries in other areas of the upper body, may have occurred and were not properly reported upon.
Ai Generated Responses to Concerns:
- Corruption in public health systems can have severe consequences, particularly in terms of access to necessary medical services and the trust people place in these systems.
- Silencing, Misdiagnosing, and False Detainment: Silencing and Discrediting: In some political systems, particularly authoritarian regimes, dissenting voices can be silenced through misdiagnosis or false labeling of mental health conditions. This can discredit individuals, making it easier to detain them without due process.
- False Detainment: Public officials may misuse their power to detain individuals under false pretenses, often using mental health diagnoses as a justification. This can be a tool to suppress political opposition or control certain populations.
Mistrust in the Medical Public Sector
- Corruption and Misuse of Funds: Corruption can lead to the misallocation of resources, resulting in inadequate healthcare services. This can erode public trust in the medical sector, as people may perceive that their health needs are not being met due to corruption.
- Lack of Transparency: When there is a lack of transparency in how healthcare funds are used, it can lead to suspicions and mistrust. People may believe that their health issues are not being addressed properly because of corrupt practices.
Limiting Access to Medical Services
- Intermediary Corruption: In many systems, access to healthcare services requires navigating through intermediaries, such as local officials or healthcare providers. If these intermediaries are corrupt, they can block access to necessary services, demanding bribes or showing favoritism.
- Geographical Barriers: In regions where healthcare services are centralized, individuals in remote areas may face significant barriers to access. Corruption can exacerbate this by diverting resources away from these areas, further limiting access.
Impact on Community Trust: Corruption erodes trust in public institutions and community cohesion. This lack of trust can exacerbate feelings of isolation and depression, as people feel unsupported by their government and community.
Further details can be found on a personal Lino Account of Codex08580, where numerous uploaded documents are placed, as all personal electronics have been taken.
By signing this petition, one recognizes and supports currently held medical ethical guidelines established by HIPAA and recognized within various treaties shown on the WMA, World Medical Associations recognized ethical medical international agreements.
Tiffany Anne Buckley (ANNE)
buckley.anne.t0880@proton.me (accessible as of 04/06/2025)
seekinglila@gmail.com (accessible as of 04/06/2025)
buckley.anne.t88@gmail.com (accessible as of 04/06/2025)
codex080580@gmail.com (not able to sign in, unable to verify w phone)
buckley.anne.t808@proton.me (not receiving emails, storage limit met)
t_anne_buckley@msn.com (not able to sign in, unable to verify)
Facebook Account Info (inaccessible for sign in as of 04/06/2025)
FB: seekinglila.truth.not.maya Tiffany Anne Buckley from Danbury, CT, GMU Fairfax, VA University Attended.
LINO ACCOUNT: CODEX08580 Username
Med Request Records - Lino Account Canvas http://linoit.com/users/codex08580/canvases/%28%28%28MedRequestRec%29%29%29
Med Fractured Humerus - Lino Account Canvas Accounthttp://linoit.com/users/codex08580/canvases/%28%28%28%29%29%29Med%20Fractured%20Humerus
This Petition is a Draft & will likely change, shortly.
Adopted by the 71st WMA General Assembly (online), Cordoba, Spain, October 2020
The relationship underwent deep changes as a result of momentous milestones such as the Universal Declaration of Human Rights (1948), the WMA declarations of Geneva (1948), Helsinki (1964), and the Lisbon (1981).The relationship has slowly progressed towards the empowerment of the patient.
Reiterating its Declaration of Geneva, the International Code of Medical Ethics and its Lisbon Declaration on Patient Rights and given the vital importance of the relationship between physician and patient in history and in the current and future context of medicine, the WMA and its
Constituent Members:
Reaffirm that professional autonomy and clinical independence are essential components of high-quality medical care and medical professionalism, protecting the right of the patients to receive the health care they need.
4. Reaffirm its opposition to interference from governments, other agents and institutional administrations in the practice of medicine and in the Patient-physician
Adopted by the 53rd WMA General Assembly, Washington, DC, USA, October 2002
and revised by the 67th WMA General Assembly, Taipei, Taiwan, October 2016
9. Respecting the dignity, autonomy, privacy and confidentiality of individuals, physicians have specific obligations, both ethical and legal, as stewards protecting information provided by their patients. The rights to autonomy, privacy and confidentiality also entitle individuals to exercise control over the use of their personal data and biological material.
Adopted by the 53rd WMA General Assembly, Washington, DC, USA, October 2002 and revised by the 67th WMA General Assembly, Taipei, Taiwan, October 2016
14. Individuals have the right to request for and be provided with information about their data and its use as well as to request corrections of mistakes or omissions. Health Databases and Biobanks should adopt adequate measures to inform the concerned individuals about their activities.
4. Health Databases and Biobanks are both collections on individuals and population, and both give rise to the similar concerns about dignity, autonomy, privacy, confidentiality and discrimination.
6. Physicians must consider the ethical, legal and regulatory norms and standards for Health Database and Biobanks in their own countries as well as applicable international norms and standards. No national or international ethical, legal or regulatory requirement should reduce or eliminate any of the protections for individuals and population set forth in this Declaration.
11. The collection, storage and use of data and biological material from individuals capable of giving consent must be voluntary. If the data and biological material are collected for a given research project, the specific, free and informed consent of the participants must be obtained in accordance with the Declaration of Helsinki.
8. Refers to the WMA Statement on Access of Women and Children to Health Care, which categorically condemns violations of the basic human right of women and children, including violations stemming from social, political, religious, economic and cultural practices.
Adopted by the 59th WMA General Assembly, Seoul, Korea, October 2008
And amended by the 69th WMA General Assembly, Reykjavik, Iceland, October 2018
Physicians recognize that they must take into account the structure of the health system and available resources when making treatment decisions. Unreasonable restraints on clinical independence imposed by governments and administrators are not in the best interests of patients because they may not be evidence based and risk undermining trust which is an essential component of the patient-physician relationship.
Adopted by the 34th World Medical Assembly, Lisbon, Portugal, September/October 1981 and amended by the 47th WMA General Assembly, Bali, Indonesia, September 1995 and editorially revised by the 171st WMA Council Session, Santiago, Chile, October 2005
and reaffirmed by the 200th WMA Council Session, Oslo, Norway, April 2015
Right to information
The patient has the right to receive information about himself/herself recorded in any of his/her medical records, and to be fully informed about his/her health status including the medical facts about his/her condition
Right to freedom of choice
The patient has the right to choose freely and change his/her physician and hospital or health service institution, regardless of whether they are based in the private or public sector.
The patient has the right to ask for the opinion of another physician at any stage.
Right to self-determination
The patient has the right to self-determination, to make free decisions regarding himself/herself. The physician will inform the patient of the consequences of his/her decisions.
A mentally competent adult patient has the right to give or withhold consent to any diagnostic procedure or therapy. The patient has the right to the information necessary to make his/her decisions. The patient should understand clearly what is the purpose of any test or treatment, what the results would imply, and what would be the implications of withholding consent.
Individuals’ Right under HIPAA to Access their Health Information 45 CFR § 164.524
Individuals have a right to access PHI in a "designated record set." A "designated record set" is defined at 45 CFR 164.501 as a group of records maintained by or for a covered entity that comprises the:
Medical records and billing records about individuals maintained by or for a covered health care provider; Enrollment, payment, claims adjudication, and case or medical management record systems maintained by or for a health plan; or
Other records that are used, in whole or in part, by or for the covered entity to make decisions about individuals. This last category includes records that are used to make decisions about any individuals, whether or not the records have been used to make a decision about the particular individual requesting access.
The term "record" means any item, collection, or grouping of information that includes PHI and is maintained, collected, used, or disseminated by or for a covered entity.
Thus, individuals have a right to a broad array of health information about themselves maintained by or for covered entities, including: medical records; billing and payment records; insurance information; clinical laboratory test results; medical images, such as X-rays; wellness and disease management program files; and clinical case notes; among other information used to make decisions about individuals. In responding to a request for access, a covered entity is not, however, required to create new information, such as explanatory materials or analyses, that does not already exist in the designated record set.

9
The Issue
Individuals’ Right under HIPAA to Access their Health Information 45 CFR § 164.524
Patients' rights are detailed in the Health Insurance Portability and Accountability Act (HIPAA) which states that individuals have a legal right to obtain copies of their health data stored by their healthcare providers.
Patient Rights – WMA – The World Medical Association
Additional Relevant Assembly Info, Located at the End Portion of this Petition.
Personal difficulties are present in gaining access to medical records, particularly of Radiology Reports & an ER report. The traditional request for records method(s) took place, returning results of "patient not found" or replies of "all records provided" with referrals to obtain in alternate ways. Technical encounters are frequent amidst, the numerous ways of which to attempt to obtain them via instruction(s) and have been reported to the associated technology companies of affiliation with the health facilities and/or practitioners.
UPMC, Pennsylvania and an additional system, VHC, Virginia are two medical networks where numerous complications of obtaining records have taken place in recent years. Despite bringing this to the attention of health regulation and standards organizations including the American Medical Association (AMA), the American Health Association (AHA), the Council for State Governments (CSG), the International Joint Commission (IJC), the World Medical Association (WMA), and United Nations affiliates, radiology reports from initial injury sustained date, have not been released.
The statute of limitations passed for the incident date of 02/05/2023 to attempt for any settlement, claims or actions. Physicians indicated within the reports, a spiral fracture of the humerus bone, yet markers indicate from the X-Rays that other areas, may have been affected and not included in the description of incidence. These photos are from 9 months post the original injury. Obtaining the ER Report from the date of incidence on 02/05/2023 and the radiology reports taken while in the state of PA, from Feb - Aug of 2023, is the reason for this request for support.
The radiology image shown here, appears to indicate injuries in other areas of the upper body, may have occurred and were not properly reported upon.
Ai Generated Responses to Concerns:
- Corruption in public health systems can have severe consequences, particularly in terms of access to necessary medical services and the trust people place in these systems.
- Silencing, Misdiagnosing, and False Detainment: Silencing and Discrediting: In some political systems, particularly authoritarian regimes, dissenting voices can be silenced through misdiagnosis or false labeling of mental health conditions. This can discredit individuals, making it easier to detain them without due process.
- False Detainment: Public officials may misuse their power to detain individuals under false pretenses, often using mental health diagnoses as a justification. This can be a tool to suppress political opposition or control certain populations.
Mistrust in the Medical Public Sector
- Corruption and Misuse of Funds: Corruption can lead to the misallocation of resources, resulting in inadequate healthcare services. This can erode public trust in the medical sector, as people may perceive that their health needs are not being met due to corruption.
- Lack of Transparency: When there is a lack of transparency in how healthcare funds are used, it can lead to suspicions and mistrust. People may believe that their health issues are not being addressed properly because of corrupt practices.
Limiting Access to Medical Services
- Intermediary Corruption: In many systems, access to healthcare services requires navigating through intermediaries, such as local officials or healthcare providers. If these intermediaries are corrupt, they can block access to necessary services, demanding bribes or showing favoritism.
- Geographical Barriers: In regions where healthcare services are centralized, individuals in remote areas may face significant barriers to access. Corruption can exacerbate this by diverting resources away from these areas, further limiting access.
Impact on Community Trust: Corruption erodes trust in public institutions and community cohesion. This lack of trust can exacerbate feelings of isolation and depression, as people feel unsupported by their government and community.
Further details can be found on a personal Lino Account of Codex08580, where numerous uploaded documents are placed, as all personal electronics have been taken.
By signing this petition, one recognizes and supports currently held medical ethical guidelines established by HIPAA and recognized within various treaties shown on the WMA, World Medical Associations recognized ethical medical international agreements.
Tiffany Anne Buckley (ANNE)
buckley.anne.t0880@proton.me (accessible as of 04/06/2025)
seekinglila@gmail.com (accessible as of 04/06/2025)
buckley.anne.t88@gmail.com (accessible as of 04/06/2025)
codex080580@gmail.com (not able to sign in, unable to verify w phone)
buckley.anne.t808@proton.me (not receiving emails, storage limit met)
t_anne_buckley@msn.com (not able to sign in, unable to verify)
Facebook Account Info (inaccessible for sign in as of 04/06/2025)
FB: seekinglila.truth.not.maya Tiffany Anne Buckley from Danbury, CT, GMU Fairfax, VA University Attended.
LINO ACCOUNT: CODEX08580 Username
Med Request Records - Lino Account Canvas http://linoit.com/users/codex08580/canvases/%28%28%28MedRequestRec%29%29%29
Med Fractured Humerus - Lino Account Canvas Accounthttp://linoit.com/users/codex08580/canvases/%28%28%28%29%29%29Med%20Fractured%20Humerus

This Petition is a Draft & will likely change, shortly.
Adopted by the 71st WMA General Assembly (online), Cordoba, Spain, October 2020
The relationship underwent deep changes as a result of momentous milestones such as the Universal Declaration of Human Rights (1948), the WMA declarations of Geneva (1948), Helsinki (1964), and the Lisbon (1981).The relationship has slowly progressed towards the empowerment of the patient.
Reiterating its Declaration of Geneva, the International Code of Medical Ethics and its Lisbon Declaration on Patient Rights and given the vital importance of the relationship between physician and patient in history and in the current and future context of medicine, the WMA and its
Constituent Members:
Reaffirm that professional autonomy and clinical independence are essential components of high-quality medical care and medical professionalism, protecting the right of the patients to receive the health care they need.
4. Reaffirm its opposition to interference from governments, other agents and institutional administrations in the practice of medicine and in the Patient-physician
Adopted by the 53rd WMA General Assembly, Washington, DC, USA, October 2002
and revised by the 67th WMA General Assembly, Taipei, Taiwan, October 2016
9. Respecting the dignity, autonomy, privacy and confidentiality of individuals, physicians have specific obligations, both ethical and legal, as stewards protecting information provided by their patients. The rights to autonomy, privacy and confidentiality also entitle individuals to exercise control over the use of their personal data and biological material.
Adopted by the 53rd WMA General Assembly, Washington, DC, USA, October 2002 and revised by the 67th WMA General Assembly, Taipei, Taiwan, October 2016
14. Individuals have the right to request for and be provided with information about their data and its use as well as to request corrections of mistakes or omissions. Health Databases and Biobanks should adopt adequate measures to inform the concerned individuals about their activities.
4. Health Databases and Biobanks are both collections on individuals and population, and both give rise to the similar concerns about dignity, autonomy, privacy, confidentiality and discrimination.
6. Physicians must consider the ethical, legal and regulatory norms and standards for Health Database and Biobanks in their own countries as well as applicable international norms and standards. No national or international ethical, legal or regulatory requirement should reduce or eliminate any of the protections for individuals and population set forth in this Declaration.
11. The collection, storage and use of data and biological material from individuals capable of giving consent must be voluntary. If the data and biological material are collected for a given research project, the specific, free and informed consent of the participants must be obtained in accordance with the Declaration of Helsinki.
8. Refers to the WMA Statement on Access of Women and Children to Health Care, which categorically condemns violations of the basic human right of women and children, including violations stemming from social, political, religious, economic and cultural practices.
Adopted by the 59th WMA General Assembly, Seoul, Korea, October 2008
And amended by the 69th WMA General Assembly, Reykjavik, Iceland, October 2018
Physicians recognize that they must take into account the structure of the health system and available resources when making treatment decisions. Unreasonable restraints on clinical independence imposed by governments and administrators are not in the best interests of patients because they may not be evidence based and risk undermining trust which is an essential component of the patient-physician relationship.
Adopted by the 34th World Medical Assembly, Lisbon, Portugal, September/October 1981 and amended by the 47th WMA General Assembly, Bali, Indonesia, September 1995 and editorially revised by the 171st WMA Council Session, Santiago, Chile, October 2005
and reaffirmed by the 200th WMA Council Session, Oslo, Norway, April 2015
Right to information
The patient has the right to receive information about himself/herself recorded in any of his/her medical records, and to be fully informed about his/her health status including the medical facts about his/her condition
Right to freedom of choice
The patient has the right to choose freely and change his/her physician and hospital or health service institution, regardless of whether they are based in the private or public sector.
The patient has the right to ask for the opinion of another physician at any stage.
Right to self-determination
The patient has the right to self-determination, to make free decisions regarding himself/herself. The physician will inform the patient of the consequences of his/her decisions.
A mentally competent adult patient has the right to give or withhold consent to any diagnostic procedure or therapy. The patient has the right to the information necessary to make his/her decisions. The patient should understand clearly what is the purpose of any test or treatment, what the results would imply, and what would be the implications of withholding consent.
Individuals’ Right under HIPAA to Access their Health Information 45 CFR § 164.524
Individuals have a right to access PHI in a "designated record set." A "designated record set" is defined at 45 CFR 164.501 as a group of records maintained by or for a covered entity that comprises the:
Medical records and billing records about individuals maintained by or for a covered health care provider; Enrollment, payment, claims adjudication, and case or medical management record systems maintained by or for a health plan; or
Other records that are used, in whole or in part, by or for the covered entity to make decisions about individuals. This last category includes records that are used to make decisions about any individuals, whether or not the records have been used to make a decision about the particular individual requesting access.
The term "record" means any item, collection, or grouping of information that includes PHI and is maintained, collected, used, or disseminated by or for a covered entity.
Thus, individuals have a right to a broad array of health information about themselves maintained by or for covered entities, including: medical records; billing and payment records; insurance information; clinical laboratory test results; medical images, such as X-rays; wellness and disease management program files; and clinical case notes; among other information used to make decisions about individuals. In responding to a request for access, a covered entity is not, however, required to create new information, such as explanatory materials or analyses, that does not already exist in the designated record set.

9
Petition Updates
Share this petition
Petition created on April 6, 2025