

Save Karen Gordon from Dying of Malnutrition and Dehydration due to NHS Failings.


Save Karen Gordon from Dying of Malnutrition and Dehydration due to NHS Failings.
The Issue
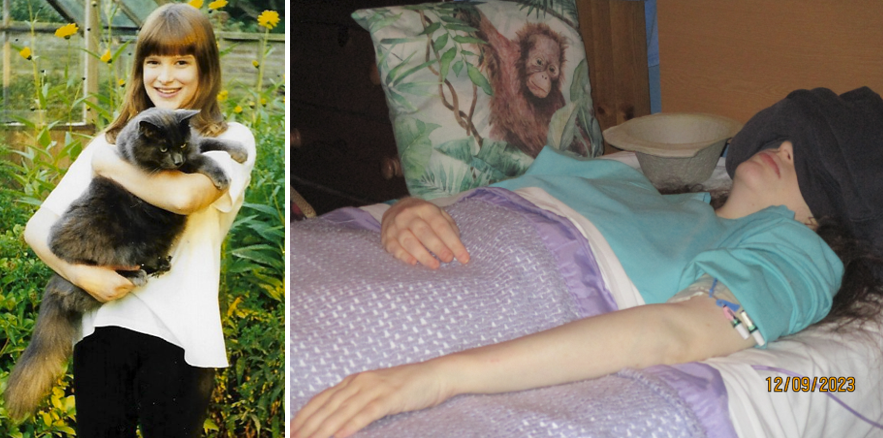
Please sign this petition to try and save Karen Gordon’s life. She is a 39-year-old lady who has very severe Myalgic Encephalomyelitis (ME). Karen lives in East Sussex, South East England.
Karen is in Conquest hospital in Hastings, East Sussex. Karen has been in hospital for more than 2 years and 5 months. She has been in hospital since the 19th of December 2023. Karen is being given TPN (IV feeding) and IV fluid. Karen needs the TPN and IV fluid to continue as she will die without them. Karen does not want to die.
Karen needs East Sussex Healthcare NHS Trust (ESHT) to make special arrangements that are suitable for Karen to facilitate for her to have TPN and IV fluid at home.
ESHT say Karen has to go to a tertiary TPN unit for assessments and possible setting up of home PN (IV feeding). However, due to Karen’s very severe ME, travelling to and being at a unit would relapse the ME and she would not be able to do all the usual assessments. Some other NHS hospitals do not require patients to go to a tertiary TPN unit. Karen needs remote setting up of home PN while she is in Conquest hospital.
ME experts support Karen’s need for remote setting up of home PN and have asked for her to be given this.
In July 2025 ESHT told Karen that they might take Karen's case to Court and try to evict Karen from hospital. This would be without TPN and IV fluid. This would be a death sentence as Karen would not survive without TPN as she cannot tolerate enough feed and water through her PEG-J feeding tube to sustain her, so Karen would die of dehydration and malnutrition.
No patient should have to die because due to their illness they cannot follow the usual practice of their NHS Trust. The Trust should find a way for a patient to be given what they need in a way that is suitable for them.
We do not think that Karen should be denied access to home PN if she does not go to a unit because of the difficulties and risks that she has because of the very severe ME. ESHT need to make home PN accessible to Karen with her very severe ME.
Karen needs to go home as soon as possible but it needs to be with home PN and IV fluid. Karen wants to get home and be at home with both of her parents and her cat.
ME/CFS is classified by the World Health Organisation as a neurological condition.
Karen is totally bed bound and cannot eat or drink.
The ME causes many symptoms including generalised pain, abdominal pain, headache, nausea and vomiting, fatigue, and hypersensitivity to sensory stimuli including, light, noise and smell. She has to keep her eyes covered.
Karen is intelligent and has many interests. She enjoys receiving cards and letters. When she is at home she loves spending time with her cat and enjoys other things including having things such as some newspaper articles and updates from some of the many animal charities that she supports read to her a bit at a time when she is able.
Karen has had ME since she was 10 years old. She has been tube fed for 20 years mostly at home. Since June 2021 her ME health has become worse, causing more severe nausea and vomiting and severe abdominal pain leading to more feeding and nutritional difficulties.
In June 2021 Karen was put on TPN. The TPN has been stopped twice for months - 7 months in 2021/2022 and 8 months in 2023 - and both of these times Karen lost a lot of weight, became very thin and had life-threatening malnutrition and dehydration.
Heather is Karen’s mother and full-time carer. Karen would not be able to manage physically or emotionally without Heather by her side 24/7 when she is in hospital, giving her the one-to-one care and support, advocacy and help with communication that she needs.
Karen needs to be given a side room for the duration of each hospital admission to help provide the best environment possible in hospital for her with her very severe ME. The National Institute for Health and Care Excellence (NICE) Guidelines on ME recommend this. Consultants at both local hospitals have supported Karen’s need for a side-room. Two ME specialists have also advised the Trust that Karen be given a side-room. Despite these things, the Trust and senior nursing management have referred to Karen’s need as a ‘preference’ and refused to give Karen a room for the duration of a 2½ week hospital stay in 2023.
Being in a 4/6 bed bay is very unsuitable for Karen and causes an increase in symptoms, unnecessary suffering, deterioration of the ME and it can cause a relapse of the ME which could be life-threatening. The sensory stimuli and busyness around her in a bay are overwhelming and exhausting for Karen and cause her more severe pain. Rest and sleep are particularly important for people with ME and they are needed for energy management which the NICE guidelines advise. In a bay, Karen gets hardly any sleep or rest due to the disturbance.
For 18 years, Heather stayed with Karen 24/7 giving her care and support each time she was in hospital on the urology unit and other wards and the hospital accepted that Karen had a clinical need for a side-room. Both these things were usual practice in Karen’s care until 2023.
When we launched the petition in September 2023 Karen was suffering from malnutrition and dehydration at home. The first point we were calling for was for Karen to be started on TPN and IV fluid without delay in a local hospital.
After many months of malnutrition, dehydration, weight loss and becoming thinner and thinner Karen was eventually admitted to Conquest hospital on the 20th of December 2023. However, this was not because the Trust Board and hospital senior nursing management had arranged to admit Karen for TPN and IV fluid as they should have done to save her life. Karen was admitted because we instigated it, as her PEG-J tube was malfunctioning. On the 19th of December 2023 we called 111 and Karen was taken by ambulance to A&E at Eastbourne District General Hospital. In A&E, Karen was started on IV fluid.
The next afternoon Karen was transferred to Conquest hospital and admitted to a 6-bed bay there. Several days later she was moved to a side room. At the time we were told that this was because of her low white cell count - rather than because of her clinical need for a side room because of her very severe ME. Heather has been staying with Karen 24/7 throughout Karen’s admission. On the 21st of December 2023 Karen was started on TPN. Karen has been continuing to receive TPN and IV fluid since then.
In November 2023 Karen was referred to St Marks Intestinal Rehabilitation Unit (IRU), but they have refused to give Karen remote setting up of home PN.
Karen has major fears and concerns about going to St Marks. St Marks is 100 miles away. Travelling to and being at the unit would cause Karen serious harm. It would relapse the very severe ME making it much worse, maybe permanently. A relapse could include paralysis and/or being unable to speak, for example. It could be life threatening. Even if the relapse was not as severe as this it would increase Karen’s symptoms and substantially reduce Karen’s quality of life, maybe permanently. St Marks IRU has a strong psychiatric approach. We are all also very concerned about St Marks attitudes towards very severe ME and that they are not accepting all of Karen's needs and limitations because of her very severe ME. St Marks are reluctant to give Karen home PN even if she did go to the unit.
ESHT and senior nursing management have shown cold uncaring attitudes, a lack of respect and compassion and disbelief of Karen’s ME illness, its symptoms and how it affects her. Their attitudes, actions and threats have caused Karen intense emotional and physical stress and suffering and make her feel scared.
We call on the CEO and Directors of East Sussex Healthcare NHS Trust and the management of Conquest Hospital Hastings and Eastbourne District General Hospital:
1) To make special arrangements that are suitable for Karen to facilitate Karen to have home TPN and IV fluid without Karen having to go to St Mark’s Hospital and without all of the usual assessment processes, as she is unable to do them because of the very severe ME.
2) To not to stop Karen’s TPN and IV fluid.
3) To accept that Karen needs her mother, Heather, her full- time carer and advocate, to be with her 24/7 while she is in hospital giving her one-to-one care and support throughout each admission.
4) To give Karen a side-room for the duration of each admission because of her very severe ME.
5) To treat Karen with compassion and respect.
Please sign this petition to try to save Karen Gordon’s life by getting her TPN and IV fluid at home and without her going to a tertiary TPN unit; by her TPN and IV fluid being continued in the meantime; and to get her the conditions she needs when in hospital.
If you’d like to read the piece we wrote when we launched our petition in September 2023 scroll down to ‘UPDATES’ and find our update that we posted on the 2nd of February 2025.
21,627
The Issue

Please sign this petition to try and save Karen Gordon’s life. She is a 39-year-old lady who has very severe Myalgic Encephalomyelitis (ME). Karen lives in East Sussex, South East England.
Karen is in Conquest hospital in Hastings, East Sussex. Karen has been in hospital for more than 2 years and 5 months. She has been in hospital since the 19th of December 2023. Karen is being given TPN (IV feeding) and IV fluid. Karen needs the TPN and IV fluid to continue as she will die without them. Karen does not want to die.
Karen needs East Sussex Healthcare NHS Trust (ESHT) to make special arrangements that are suitable for Karen to facilitate for her to have TPN and IV fluid at home.
ESHT say Karen has to go to a tertiary TPN unit for assessments and possible setting up of home PN (IV feeding). However, due to Karen’s very severe ME, travelling to and being at a unit would relapse the ME and she would not be able to do all the usual assessments. Some other NHS hospitals do not require patients to go to a tertiary TPN unit. Karen needs remote setting up of home PN while she is in Conquest hospital.
ME experts support Karen’s need for remote setting up of home PN and have asked for her to be given this.
In July 2025 ESHT told Karen that they might take Karen's case to Court and try to evict Karen from hospital. This would be without TPN and IV fluid. This would be a death sentence as Karen would not survive without TPN as she cannot tolerate enough feed and water through her PEG-J feeding tube to sustain her, so Karen would die of dehydration and malnutrition.
No patient should have to die because due to their illness they cannot follow the usual practice of their NHS Trust. The Trust should find a way for a patient to be given what they need in a way that is suitable for them.
We do not think that Karen should be denied access to home PN if she does not go to a unit because of the difficulties and risks that she has because of the very severe ME. ESHT need to make home PN accessible to Karen with her very severe ME.
Karen needs to go home as soon as possible but it needs to be with home PN and IV fluid. Karen wants to get home and be at home with both of her parents and her cat.
ME/CFS is classified by the World Health Organisation as a neurological condition.
Karen is totally bed bound and cannot eat or drink.
The ME causes many symptoms including generalised pain, abdominal pain, headache, nausea and vomiting, fatigue, and hypersensitivity to sensory stimuli including, light, noise and smell. She has to keep her eyes covered.
Karen is intelligent and has many interests. She enjoys receiving cards and letters. When she is at home she loves spending time with her cat and enjoys other things including having things such as some newspaper articles and updates from some of the many animal charities that she supports read to her a bit at a time when she is able.
Karen has had ME since she was 10 years old. She has been tube fed for 20 years mostly at home. Since June 2021 her ME health has become worse, causing more severe nausea and vomiting and severe abdominal pain leading to more feeding and nutritional difficulties.
In June 2021 Karen was put on TPN. The TPN has been stopped twice for months - 7 months in 2021/2022 and 8 months in 2023 - and both of these times Karen lost a lot of weight, became very thin and had life-threatening malnutrition and dehydration.
Heather is Karen’s mother and full-time carer. Karen would not be able to manage physically or emotionally without Heather by her side 24/7 when she is in hospital, giving her the one-to-one care and support, advocacy and help with communication that she needs.
Karen needs to be given a side room for the duration of each hospital admission to help provide the best environment possible in hospital for her with her very severe ME. The National Institute for Health and Care Excellence (NICE) Guidelines on ME recommend this. Consultants at both local hospitals have supported Karen’s need for a side-room. Two ME specialists have also advised the Trust that Karen be given a side-room. Despite these things, the Trust and senior nursing management have referred to Karen’s need as a ‘preference’ and refused to give Karen a room for the duration of a 2½ week hospital stay in 2023.
Being in a 4/6 bed bay is very unsuitable for Karen and causes an increase in symptoms, unnecessary suffering, deterioration of the ME and it can cause a relapse of the ME which could be life-threatening. The sensory stimuli and busyness around her in a bay are overwhelming and exhausting for Karen and cause her more severe pain. Rest and sleep are particularly important for people with ME and they are needed for energy management which the NICE guidelines advise. In a bay, Karen gets hardly any sleep or rest due to the disturbance.
For 18 years, Heather stayed with Karen 24/7 giving her care and support each time she was in hospital on the urology unit and other wards and the hospital accepted that Karen had a clinical need for a side-room. Both these things were usual practice in Karen’s care until 2023.
When we launched the petition in September 2023 Karen was suffering from malnutrition and dehydration at home. The first point we were calling for was for Karen to be started on TPN and IV fluid without delay in a local hospital.
After many months of malnutrition, dehydration, weight loss and becoming thinner and thinner Karen was eventually admitted to Conquest hospital on the 20th of December 2023. However, this was not because the Trust Board and hospital senior nursing management had arranged to admit Karen for TPN and IV fluid as they should have done to save her life. Karen was admitted because we instigated it, as her PEG-J tube was malfunctioning. On the 19th of December 2023 we called 111 and Karen was taken by ambulance to A&E at Eastbourne District General Hospital. In A&E, Karen was started on IV fluid.
The next afternoon Karen was transferred to Conquest hospital and admitted to a 6-bed bay there. Several days later she was moved to a side room. At the time we were told that this was because of her low white cell count - rather than because of her clinical need for a side room because of her very severe ME. Heather has been staying with Karen 24/7 throughout Karen’s admission. On the 21st of December 2023 Karen was started on TPN. Karen has been continuing to receive TPN and IV fluid since then.
In November 2023 Karen was referred to St Marks Intestinal Rehabilitation Unit (IRU), but they have refused to give Karen remote setting up of home PN.
Karen has major fears and concerns about going to St Marks. St Marks is 100 miles away. Travelling to and being at the unit would cause Karen serious harm. It would relapse the very severe ME making it much worse, maybe permanently. A relapse could include paralysis and/or being unable to speak, for example. It could be life threatening. Even if the relapse was not as severe as this it would increase Karen’s symptoms and substantially reduce Karen’s quality of life, maybe permanently. St Marks IRU has a strong psychiatric approach. We are all also very concerned about St Marks attitudes towards very severe ME and that they are not accepting all of Karen's needs and limitations because of her very severe ME. St Marks are reluctant to give Karen home PN even if she did go to the unit.
ESHT and senior nursing management have shown cold uncaring attitudes, a lack of respect and compassion and disbelief of Karen’s ME illness, its symptoms and how it affects her. Their attitudes, actions and threats have caused Karen intense emotional and physical stress and suffering and make her feel scared.
We call on the CEO and Directors of East Sussex Healthcare NHS Trust and the management of Conquest Hospital Hastings and Eastbourne District General Hospital:
1) To make special arrangements that are suitable for Karen to facilitate Karen to have home TPN and IV fluid without Karen having to go to St Mark’s Hospital and without all of the usual assessment processes, as she is unable to do them because of the very severe ME.
2) To not to stop Karen’s TPN and IV fluid.
3) To accept that Karen needs her mother, Heather, her full- time carer and advocate, to be with her 24/7 while she is in hospital giving her one-to-one care and support throughout each admission.
4) To give Karen a side-room for the duration of each admission because of her very severe ME.
5) To treat Karen with compassion and respect.
Please sign this petition to try to save Karen Gordon’s life by getting her TPN and IV fluid at home and without her going to a tertiary TPN unit; by her TPN and IV fluid being continued in the meantime; and to get her the conditions she needs when in hospital.
If you’d like to read the piece we wrote when we launched our petition in September 2023 scroll down to ‘UPDATES’ and find our update that we posted on the 2nd of February 2025.
21,627
The Decision Makers
Supporter Voices
Petition Updates
Share this petition
Petition created on 14 September 2023