Make APS Testing Routine in Pregnancy to Prevent Heartbreaking Loss


Make APS Testing Routine in Pregnancy to Prevent Heartbreaking Loss
The Issue
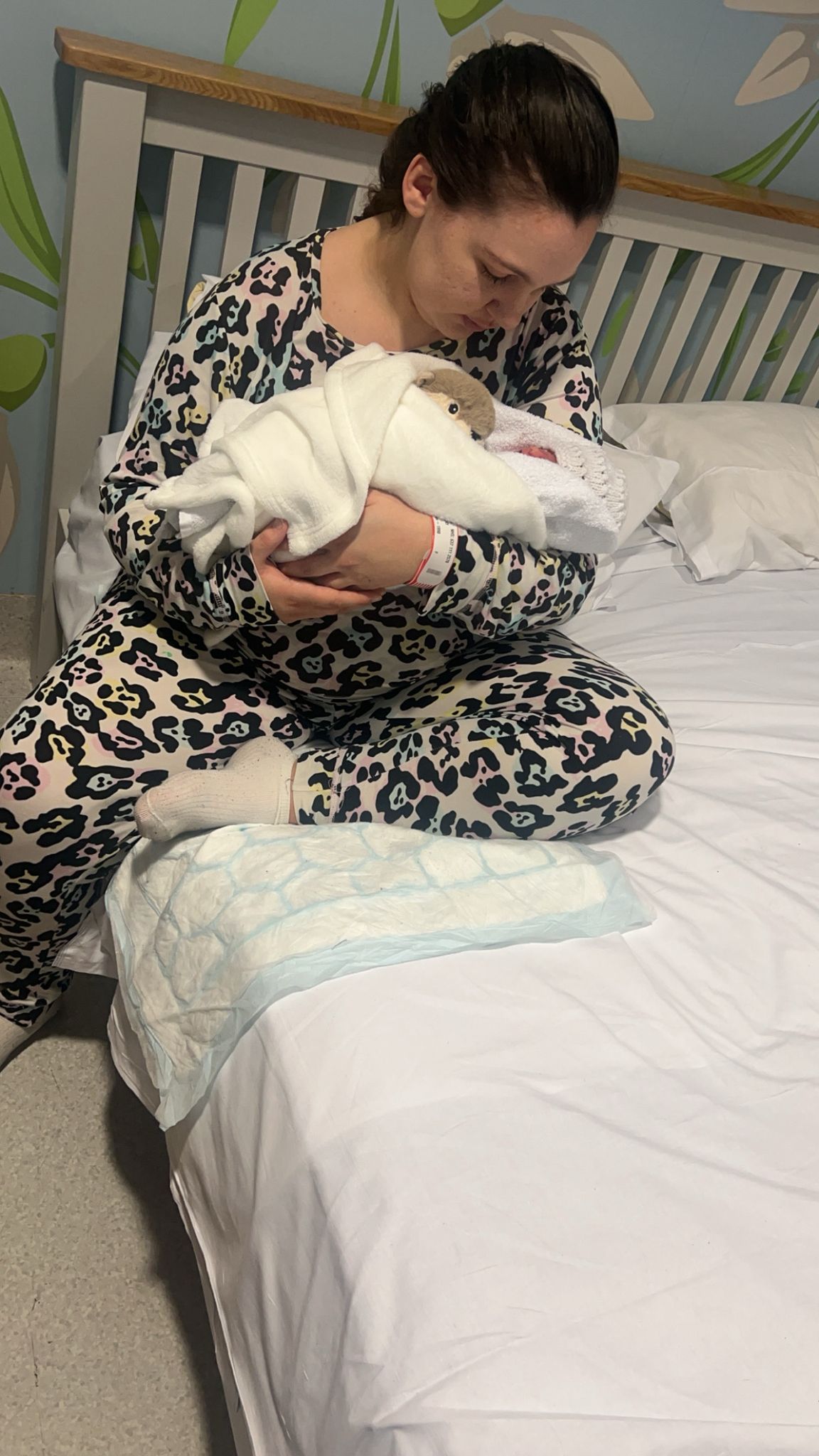
My name is Laura, and on January 15th, 2025, my beautiful daughter Rhylie was stillborn at 36 weeks. I carried her for nearly nine months, felt her kicks, dreamt of her future, and prepared to bring her home. But instead of holding her in life, I had to hold her in silence — and then say goodbye.
After her birth, I was tested for Antiphospholipid Syndrome (APS) — a condition that increases the risk of blood clots, pre-eclampsia, placental failure, and stillbirth. I received a positive result. I am still waiting for my 12-week postnatal confirmation test, but I already know deep down what it will say.
My placenta had been deteriorating for weeks, slowly failing, and no one knew. If APS had been tested for and treated earlier, my daughter might still be here. I would be holding her now, not visiting her grave.
And I am not alone.
Just weeks after I lost Rhylie, my friend Chloe gave birth to her son Hudson — and he, too, was stillborn on February 11th, 2025. He left behind three big sisters, aged 6, 3, and just 1 and a half. They were so excited to meet him. Now they’re growing up with grief too big for their little hearts to carry.
Too many families are being destroyed by silent, preventable conditions like APS. These are not rare stories — but they are being routinely missed, dismissed, and ignored.
I was due to be referred for IVF in August 2024, after years of fertility struggles and PCOS. But by then, I was already pregnant — and we were overjoyed. Rhylie was my miracle baby. She was healthy. I did everything I could. But it still wasn’t enough — because I wasn’t tested for APS.
Currently, the NHS only tests for APS after multiple miscarriages, stillbirth, or clear clotting problems. This means many women who have APS are never tested early enough, sometimes only after heartbreaking losses. There are several reasons for this:
Testing every pregnant woman or after a single miscarriage requires many blood tests and follow-ups, and the NHS must balance cost and resources.
NHS guidelines focus on women with repeated pregnancy losses or known risk factors, so early routine screening isn’t standard practice.
Diagnosing APS is complex, requiring multiple blood tests over time.
Broad screening risks false positives, which can cause unnecessary anxiety or treatment.
While these reasons exist, they mean many families suffer preventable losses because APS isn’t detected in time. Women like me show that earlier and routine APS screening during pregnancy — and even after a single miscarriage — could save lives and prevent unbearable grief. Testing should happen before a miscarriage because APS could be the reason someone doesn’t get to bring their baby home.
I am urging the NHS throughout the UK, the Scottish Government, and the UK Department of Health and Social Care to:
- Make APS screening routine early in pregnancy for all women.
Test for APS after a single miscarriage, not only after multiple losses. - Raise awareness among healthcare professionals and pregnant women about APS risks.
- Provide timely, consistent monitoring and treatment for women diagnosed with APS.
Early diagnosis and treatment — often just with aspirin and blood thinners — can save lives.
This pain is unbearable. But it’s even harder knowing it didn’t have to happen.
This isn’t about one baby. It’s about hundreds of babies, thousands of grieving parents, and a healthcare system that must do better.
No more empty cots.
No more silent delivery rooms.
No more mothers like me or Chloe walking out of hospitals with only memories.
Please sign this petition and help us make change — so that Rhylie, Hudson, and all the babies lost too soon didn’t die in vain.

618
The Issue
My name is Laura, and on January 15th, 2025, my beautiful daughter Rhylie was stillborn at 36 weeks. I carried her for nearly nine months, felt her kicks, dreamt of her future, and prepared to bring her home. But instead of holding her in life, I had to hold her in silence — and then say goodbye.
After her birth, I was tested for Antiphospholipid Syndrome (APS) — a condition that increases the risk of blood clots, pre-eclampsia, placental failure, and stillbirth. I received a positive result. I am still waiting for my 12-week postnatal confirmation test, but I already know deep down what it will say.
My placenta had been deteriorating for weeks, slowly failing, and no one knew. If APS had been tested for and treated earlier, my daughter might still be here. I would be holding her now, not visiting her grave.
And I am not alone.
Just weeks after I lost Rhylie, my friend Chloe gave birth to her son Hudson — and he, too, was stillborn on February 11th, 2025. He left behind three big sisters, aged 6, 3, and just 1 and a half. They were so excited to meet him. Now they’re growing up with grief too big for their little hearts to carry.

Too many families are being destroyed by silent, preventable conditions like APS. These are not rare stories — but they are being routinely missed, dismissed, and ignored.
I was due to be referred for IVF in August 2024, after years of fertility struggles and PCOS. But by then, I was already pregnant — and we were overjoyed. Rhylie was my miracle baby. She was healthy. I did everything I could. But it still wasn’t enough — because I wasn’t tested for APS.
Currently, the NHS only tests for APS after multiple miscarriages, stillbirth, or clear clotting problems. This means many women who have APS are never tested early enough, sometimes only after heartbreaking losses. There are several reasons for this:
Testing every pregnant woman or after a single miscarriage requires many blood tests and follow-ups, and the NHS must balance cost and resources.
NHS guidelines focus on women with repeated pregnancy losses or known risk factors, so early routine screening isn’t standard practice.
Diagnosing APS is complex, requiring multiple blood tests over time.
Broad screening risks false positives, which can cause unnecessary anxiety or treatment.
While these reasons exist, they mean many families suffer preventable losses because APS isn’t detected in time. Women like me show that earlier and routine APS screening during pregnancy — and even after a single miscarriage — could save lives and prevent unbearable grief. Testing should happen before a miscarriage because APS could be the reason someone doesn’t get to bring their baby home.
I am urging the NHS throughout the UK, the Scottish Government, and the UK Department of Health and Social Care to:
- Make APS screening routine early in pregnancy for all women.
Test for APS after a single miscarriage, not only after multiple losses. - Raise awareness among healthcare professionals and pregnant women about APS risks.
- Provide timely, consistent monitoring and treatment for women diagnosed with APS.
Early diagnosis and treatment — often just with aspirin and blood thinners — can save lives.
This pain is unbearable. But it’s even harder knowing it didn’t have to happen.
This isn’t about one baby. It’s about hundreds of babies, thousands of grieving parents, and a healthcare system that must do better.
No more empty cots.
No more silent delivery rooms.
No more mothers like me or Chloe walking out of hospitals with only memories.
Please sign this petition and help us make change — so that Rhylie, Hudson, and all the babies lost too soon didn’t die in vain.

618
The Decision Makers
Supporter Voices
Petition Updates
Share this petition
Petition created on 9 June 2025