China: Parents Call for an Independent Judicial Investigation After a Five-Month-Old Infan


China: Parents Call for an Independent Judicial Investigation After a Five-Month-Old Infan
The issue
This is LuoXi’s story
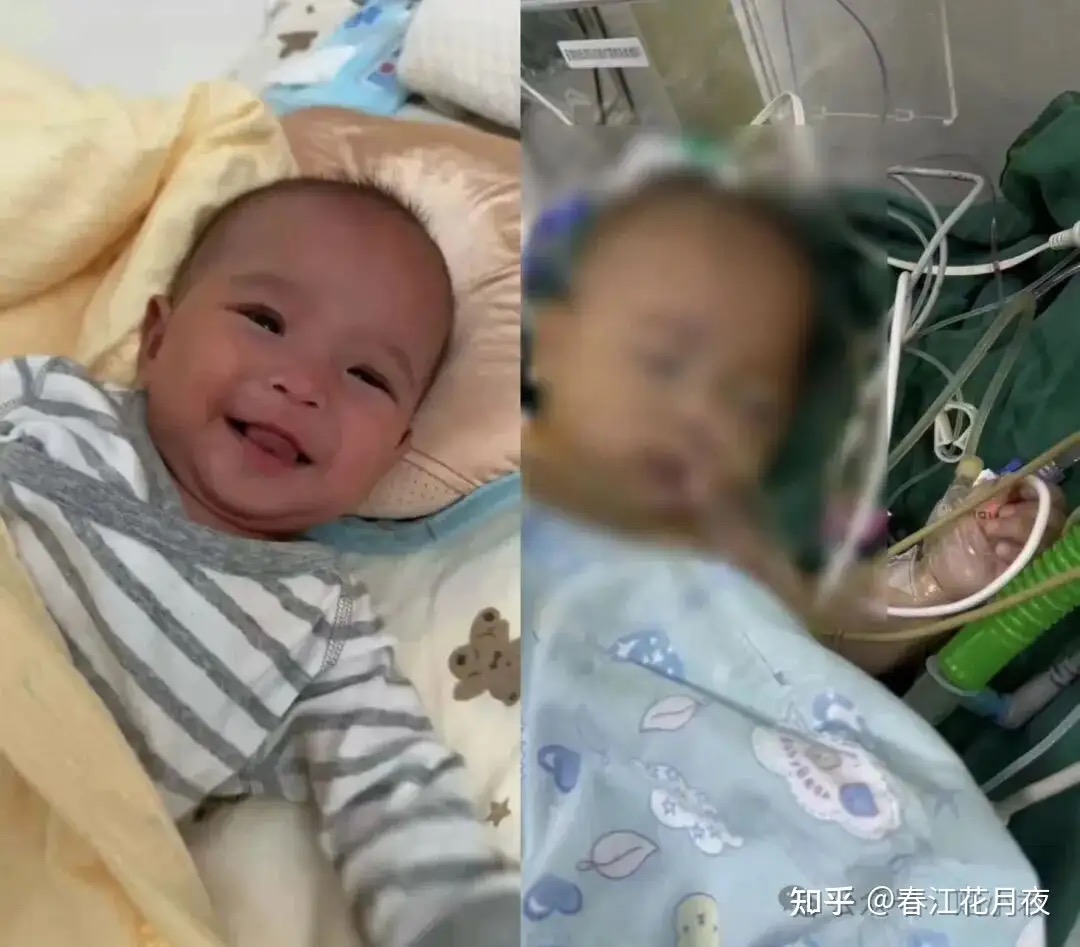
A five-month-old premature baby girl who died during what her parents were told would be a safe, minimally invasive heart surgery lasting only 2–3 hours.
Her name is LuoXi.

1. From a routine check-up to “urgent surgery”
On 11 November 2025, LuoXi attended a routine physical examination.
Although she was born prematurely, she had been developing well, and all previous check-ups were normal.
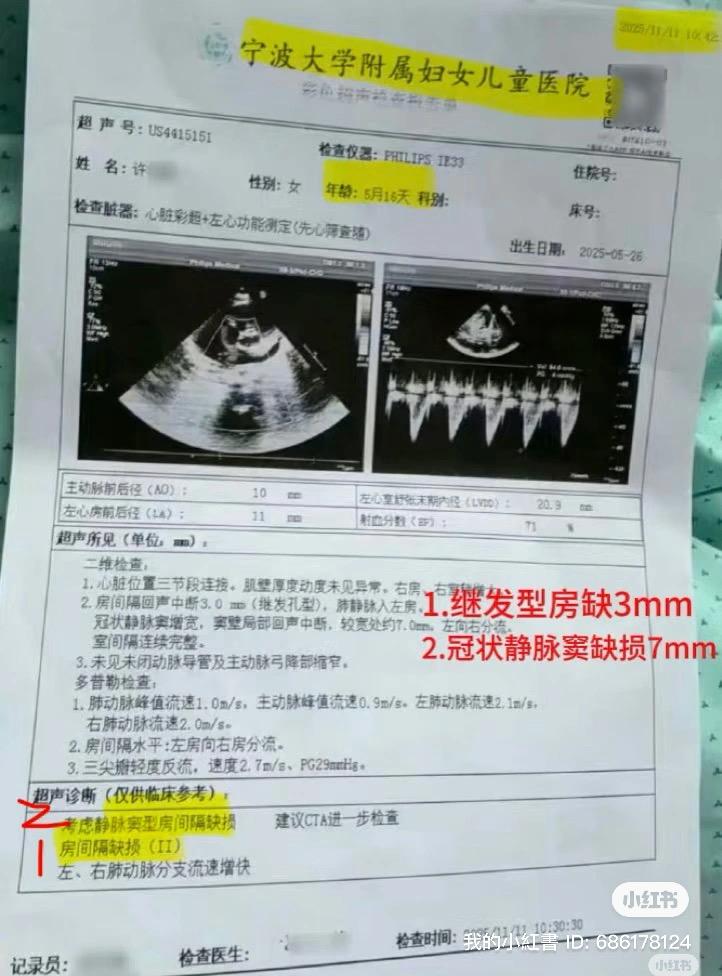
During this visit, a cardiac ultrasound was performed. Doctors told the family that two findings were identified:
A ~3 mm secundum atrial septal defect (ASD)
A ~7 mm unroofed coronary sinus (UCS)
Doctors repeatedly warned the parents that without immediate surgery, the baby could suffer:
Impaired brain development
Restricted lung development
Feeding difficulties
Serious long-term health consequences
They were told again and again: “The earlier the surgery, the better.”
However, the parents were not informed of the following critical medical facts:
Secundum atrial septal defects (ASD) are among the most common congenital heart findings in infants;
Small secundum ASDs (such as 3 mm) often close spontaneously within the first 6–12 months of life, and do not necessarily require immediate surgery;
Unroofed coronary sinus (UCS) is a rare cardiac anomaly, and the decision to operate requires further detailed imaging (such as transesophageal echocardiography, TEE) — a single routine transthoracic ultrasound is insufficient to justify emergency surgery.
These options — including observation and follow-up — were never clearly explained.
Under intense pressure, the parents signed a consent form for what was described as:
A minimally invasive repair through a small incision under the arm
Expected duration: 2–3 hours
They did not know that the baby’s chest would later be opened twice, and that the nature and risk level of the surgery would be fundamentally changed.
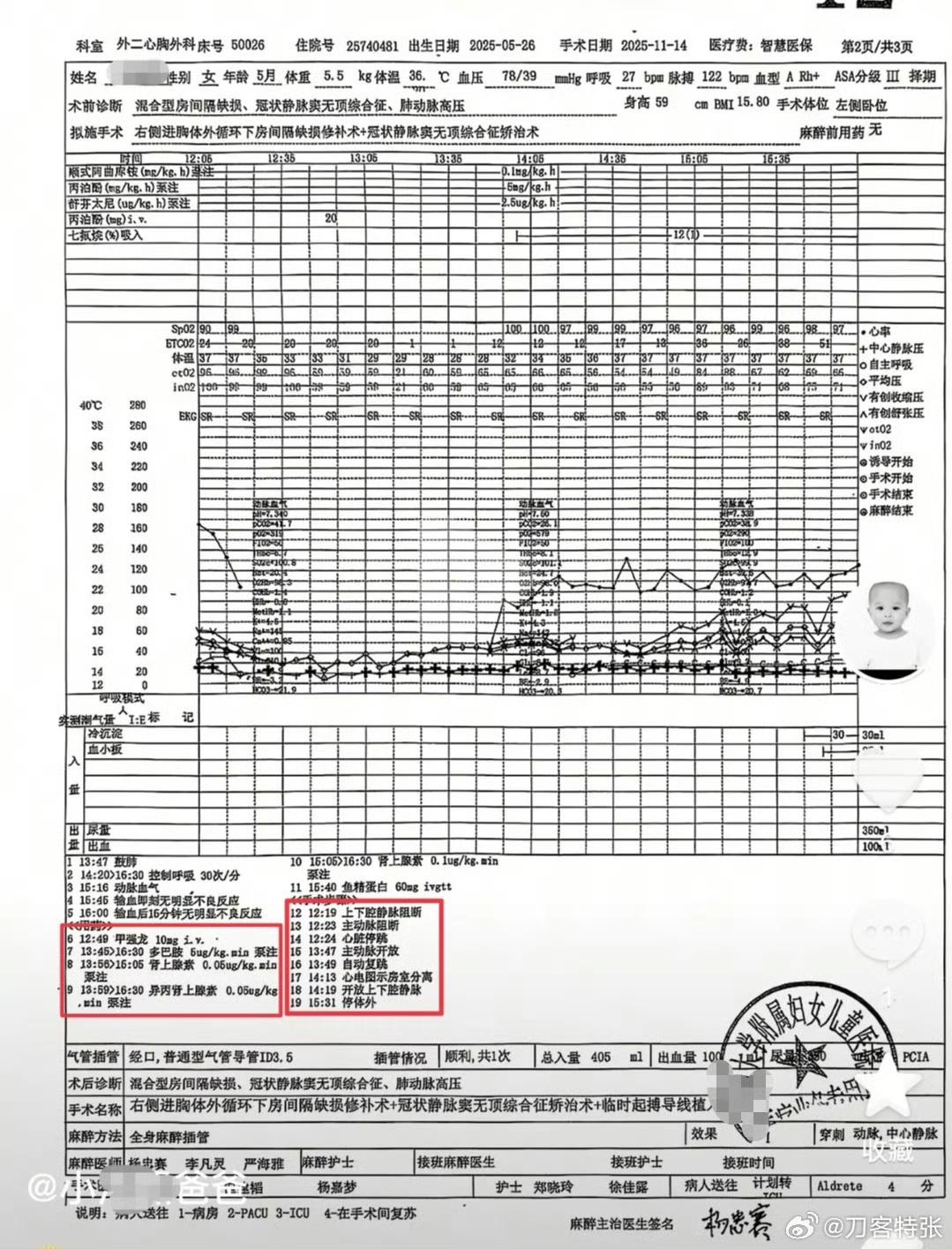
2. Surgery day: major changes without consent
14 November 2025 – Ningbo, China
07:48 – LuoXi entered the operating room
(After prolonged fasting and repeated blood draws; the additional risks to a premature infant were never explained)
09:25 – Surgery officially began
Planned as a minimally invasive procedure, without open-chest surgery
Around 11:00 – Serious problems occurred
The family was not informed
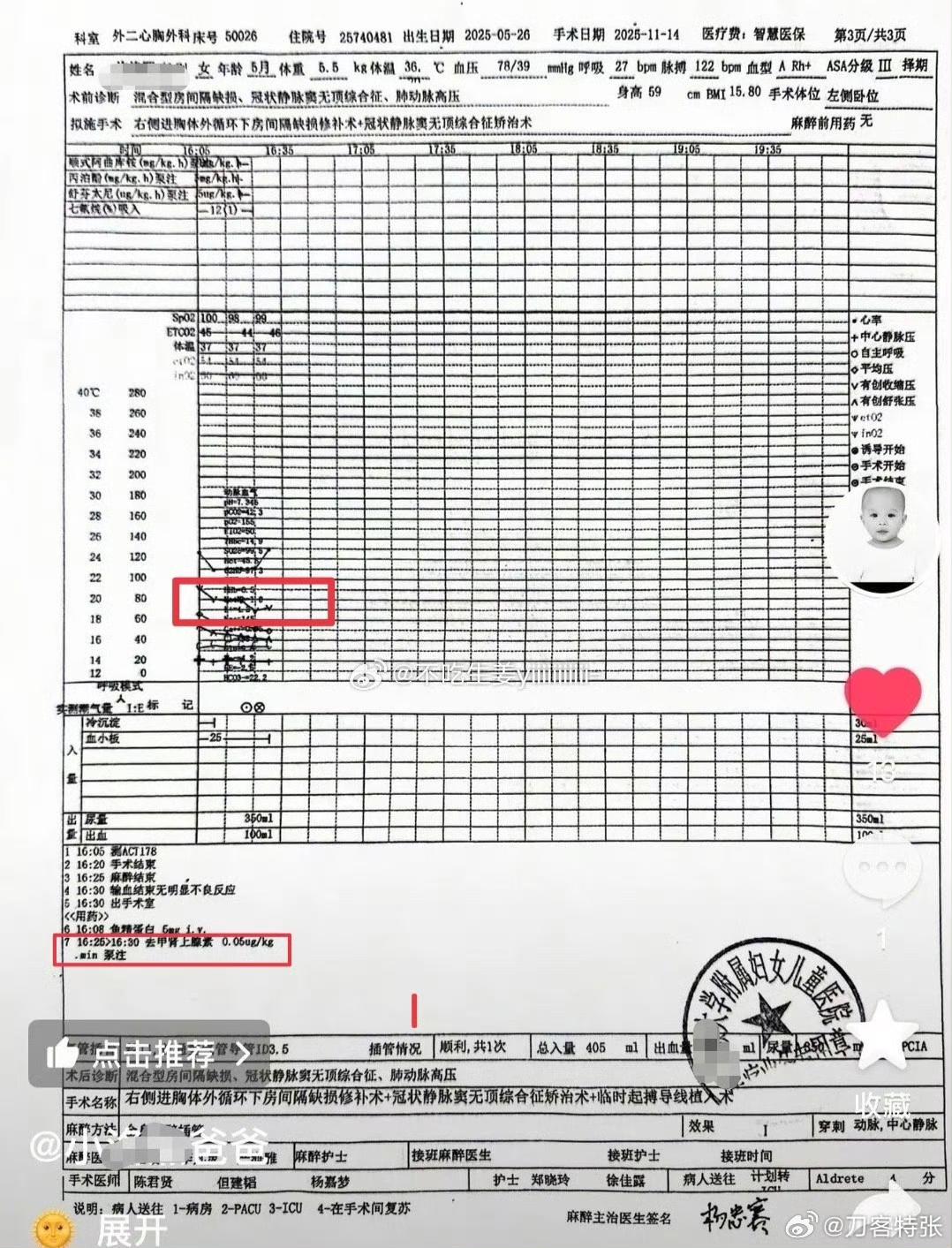
13:00–14:30 –
The surgery was escalated to open-chest surgery, and later opened again
👉 No renewed consent was obtained
16:00 –
Doctors told the family for the first time:
“There were difficulties. The child has a 50% risk.”
16:37 –
LuoXi was brought out of the operating room
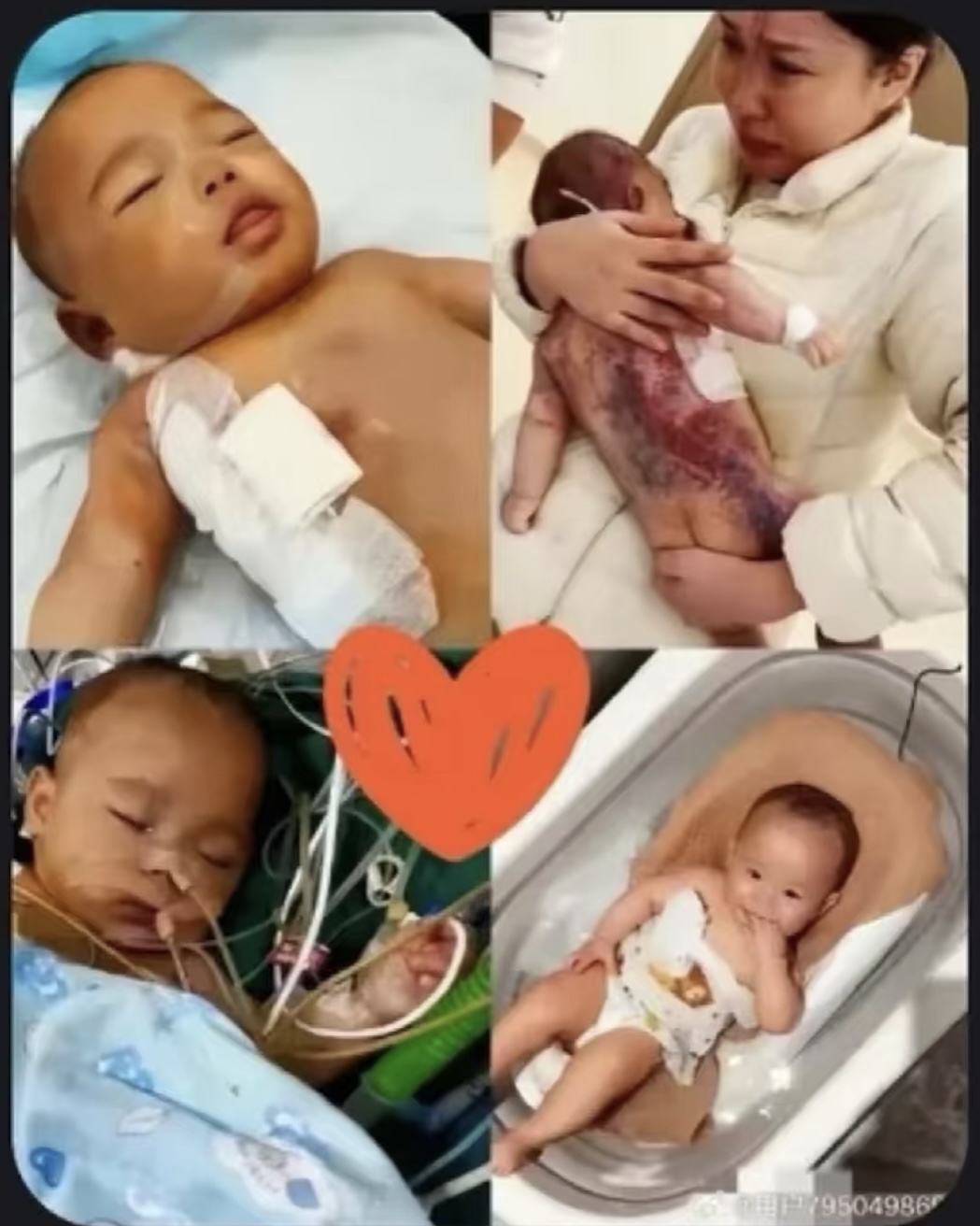
Her face was purple and swollen, and she showed no response
Yet doctors told the parents:
“The surgery went very well.”
3. PICU: repeatedly told “stable,” but she never woke up
After being transferred to the PICU, the parents were repeatedly denied access.
Doctors continued to reassure them:
“The surgery was successful. We just need to observe.”
However, during brief and restricted glimpses, the parents saw:
Severe swelling and bruising
Multiple tubes
An incompletely closed wound
No response to external stimuli
They later learned that multiple medications were required to maintain her vital signs.
4. Contradictions in the time of death
21:05 – The family later learned that the baby had no vital signs
22:03 – The hospital officially declared death
22:20 – Medical records still stated: “vital signs stable”
The mother was allowed to hold her child eight hours after the official declaration of death.
Before that, the five-month-old baby lay naked on a diaper pad throughout the night.
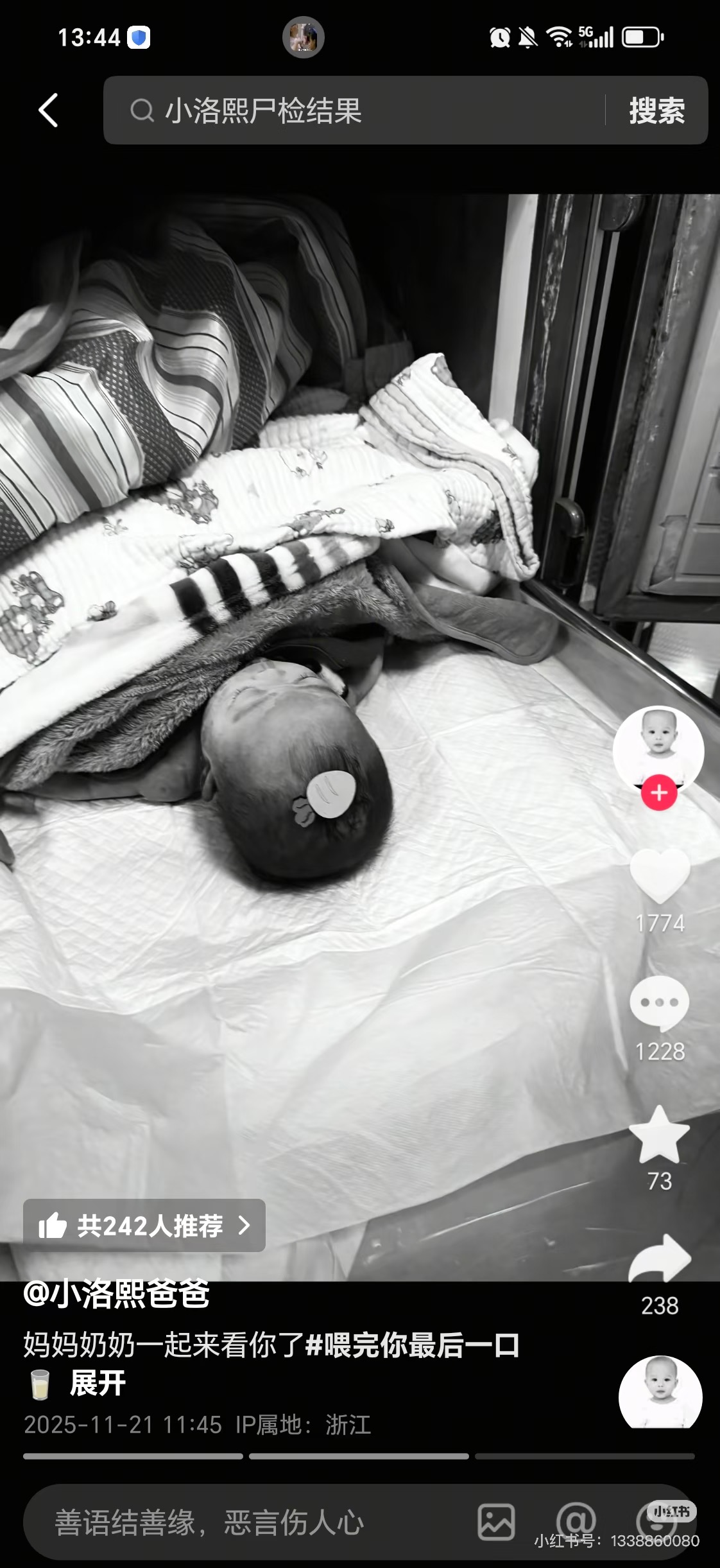
5. Critical medical evidence withheld
The family formally requested the following materials. All requests were denied with the explanation that they “do not exist or cannot be provided”:
Intraoperative video recordings
Records documenting surgical plan changes
ICU resuscitation footage
The hospital further stated that:
Operating room surveillance has no playback function
Key hard drives are missing
Pre-operative and intra-operative TEE reports were refused
Only a single post-operative report was provided
6. Autopsy findings (please read carefully)
On 20 December 2025, the family released the autopsy report, which revealed:
No 7 mm unroofed coronary sinus defect
The heart did not meet surgical indications
The cause of death was intracardiac hemorrhage directly related to surgical intervention
Findings included unclosed cardiac incisions, retained patch material, and multiple unsutured wounds
These findings directly contradict the hospital’s claim that the surgery was “successful” and that death was due to “post-operative complications.”
7. Official notice failed to address core issues
On 18 December 2025, the local health authority released an administrative notice stating:
“Insufficient pre-operative assessment”
Administrative penalties were issued
However:
No doctors were named
Key contradictions were not explained
The notice continued to assert that the baby “met surgical indications” and that the surgeon was “qualified”
The autopsy findings remain unaddressed.
8. Official Responses Raise Further Concerns
On 5 January 2026, the Ningbo Health Commission stated that:
the medical records were merely “poorly written,” not inaccurate;
leaving surgical wounds unsutured was “normal clinical practice,” and hospitals are permitted not to close incisions;
the absence of key records, including missing documentation and refusal to provide TEE reports, was due to “institutional differences” and therefore outside regulatory intervention.
These explanations do not address the autopsy findings or the missing evidence.
The family has now filed an administrative lawsuit against the Health Commission.
Despite this, the Health Commission has announced its intention to unilaterally initiate a medical accident appraisal process, without the family’s consent and despite ongoing legal proceedings and court involvement.
The family fears that such a process — conducted within the same local administrative system — cannot provide an independent or transparent determination of responsibility.
Our requests
We do not presume guilt.
We respectfully ask for:
Our Requests
We do not presume guilt.
We respectfully call for:
“an independent judicial investigation, separate from the hospital and local administrative authorities;”
full disclosure of all original medical records and data;
a truthful reconstruction of how LuoXi died;
safeguards to protect other children from similar harm.
When parents are denied the right to know how their child died,
this is not only a family tragedy —
it is a warning about the safety of all children.
Please stand for truth.
Please stand for children’s lives.
More details ,please visit our website for "LuoXi"
https://www.the-little-star.org/?lang=en




3,246
The issue
This is LuoXi’s story
A five-month-old premature baby girl who died during what her parents were told would be a safe, minimally invasive heart surgery lasting only 2–3 hours.
Her name is LuoXi.

1. From a routine check-up to “urgent surgery”
On 11 November 2025, LuoXi attended a routine physical examination.
Although she was born prematurely, she had been developing well, and all previous check-ups were normal.
During this visit, a cardiac ultrasound was performed. Doctors told the family that two findings were identified:
A ~3 mm secundum atrial septal defect (ASD)
A ~7 mm unroofed coronary sinus (UCS)
Doctors repeatedly warned the parents that without immediate surgery, the baby could suffer:
Impaired brain development
Restricted lung development
Feeding difficulties
Serious long-term health consequences
They were told again and again: “The earlier the surgery, the better.”
However, the parents were not informed of the following critical medical facts:
Secundum atrial septal defects (ASD) are among the most common congenital heart findings in infants;
Small secundum ASDs (such as 3 mm) often close spontaneously within the first 6–12 months of life, and do not necessarily require immediate surgery;
Unroofed coronary sinus (UCS) is a rare cardiac anomaly, and the decision to operate requires further detailed imaging (such as transesophageal echocardiography, TEE) — a single routine transthoracic ultrasound is insufficient to justify emergency surgery.
These options — including observation and follow-up — were never clearly explained.
Under intense pressure, the parents signed a consent form for what was described as:
A minimally invasive repair through a small incision under the arm
Expected duration: 2–3 hours
They did not know that the baby’s chest would later be opened twice, and that the nature and risk level of the surgery would be fundamentally changed.
2. Surgery day: major changes without consent
14 November 2025 – Ningbo, China
07:48 – LuoXi entered the operating room
(After prolonged fasting and repeated blood draws; the additional risks to a premature infant were never explained)
09:25 – Surgery officially began
Planned as a minimally invasive procedure, without open-chest surgery
Around 11:00 – Serious problems occurred
The family was not informed
13:00–14:30 –
The surgery was escalated to open-chest surgery, and later opened again
👉 No renewed consent was obtained
16:00 –
Doctors told the family for the first time:
“There were difficulties. The child has a 50% risk.”
16:37 –
LuoXi was brought out of the operating room
Her face was purple and swollen, and she showed no response
Yet doctors told the parents:
“The surgery went very well.”
3. PICU: repeatedly told “stable,” but she never woke up
After being transferred to the PICU, the parents were repeatedly denied access.
Doctors continued to reassure them:
“The surgery was successful. We just need to observe.”
However, during brief and restricted glimpses, the parents saw:
Severe swelling and bruising
Multiple tubes
An incompletely closed wound
No response to external stimuli
They later learned that multiple medications were required to maintain her vital signs.
4. Contradictions in the time of death
21:05 – The family later learned that the baby had no vital signs
22:03 – The hospital officially declared death
22:20 – Medical records still stated: “vital signs stable”
The mother was allowed to hold her child eight hours after the official declaration of death.
Before that, the five-month-old baby lay naked on a diaper pad throughout the night.


5. Critical medical evidence withheld
The family formally requested the following materials. All requests were denied with the explanation that they “do not exist or cannot be provided”:
Intraoperative video recordings
Records documenting surgical plan changes
ICU resuscitation footage
The hospital further stated that:
Operating room surveillance has no playback function
Key hard drives are missing
Pre-operative and intra-operative TEE reports were refused
Only a single post-operative report was provided
6. Autopsy findings (please read carefully)
On 20 December 2025, the family released the autopsy report, which revealed:
No 7 mm unroofed coronary sinus defect
The heart did not meet surgical indications
The cause of death was intracardiac hemorrhage directly related to surgical intervention
Findings included unclosed cardiac incisions, retained patch material, and multiple unsutured wounds
These findings directly contradict the hospital’s claim that the surgery was “successful” and that death was due to “post-operative complications.”
7. Official notice failed to address core issues
On 18 December 2025, the local health authority released an administrative notice stating:
“Insufficient pre-operative assessment”
Administrative penalties were issued
However:
No doctors were named
Key contradictions were not explained
The notice continued to assert that the baby “met surgical indications” and that the surgeon was “qualified”
The autopsy findings remain unaddressed.
8. Official Responses Raise Further Concerns
On 5 January 2026, the Ningbo Health Commission stated that:
the medical records were merely “poorly written,” not inaccurate;
leaving surgical wounds unsutured was “normal clinical practice,” and hospitals are permitted not to close incisions;
the absence of key records, including missing documentation and refusal to provide TEE reports, was due to “institutional differences” and therefore outside regulatory intervention.
These explanations do not address the autopsy findings or the missing evidence.
The family has now filed an administrative lawsuit against the Health Commission.
Despite this, the Health Commission has announced its intention to unilaterally initiate a medical accident appraisal process, without the family’s consent and despite ongoing legal proceedings and court involvement.
The family fears that such a process — conducted within the same local administrative system — cannot provide an independent or transparent determination of responsibility.
Our requests
We do not presume guilt.
We respectfully ask for:
Our Requests
We do not presume guilt.
We respectfully call for:
“an independent judicial investigation, separate from the hospital and local administrative authorities;”
full disclosure of all original medical records and data;
a truthful reconstruction of how LuoXi died;
safeguards to protect other children from similar harm.
When parents are denied the right to know how their child died,
this is not only a family tragedy —
it is a warning about the safety of all children.
Please stand for truth.
Please stand for children’s lives.
More details ,please visit our website for "LuoXi"
https://www.the-little-star.org/?lang=en







3,246
Supporter voices
Petition created on 19 November 2025